The use of the Enhanced Recovery After Surgery (ERAS) protocol is becoming more widespread in various surgical specialties including colorectal surgery. ERAS is a multimodal perioperative approach that aims to reduce organ dysfunction and the stress response, thereby cutting down patient morbidity and duration of hospital stay. The care pathway consists of a structured series of interventions, with patient adherence essential to the success of the process (Miller et al, 2017).
In the context of stoma care, this has led to a shift in traditional approaches, in which the stoma care nurse (SCN) historically played a central role in patient education. One of the SCN's primary responsibilities is to provide comprehensive education about stoma management, which involves ensuring that patients understand fully how to care for their stoma, including ensuring that they have the practical skills and knowledge necessary for daily maintenance. The SCN also serves as the patient's guide through the complexities of the healthcare system, ensuring that their individual care needs are addressed effectively. This advocacy role is essential in helping patients navigate their care journey and to promote their overall wellbeing.
Additionally, the SCN is responsible for supporting the discharge planning process. This includes providing and scheduling follow-up appointments to ensure continuity of support after the patient leaves hospital.
However, new professional roles are emerging in response to the development of personalised care models. One of these roles is that of the case manager (CM); this is a key role that involves having oversight of a patient's entire care pathway. The CM works in co-ordination with other health professionals to ensure a smooth transition between the different phases of care, and to maintain continuity of care at a high standard. The role is crucial for providing consistent care as patients move from hospital to home, ensuring uninterrupted treatment plans. It has been suggested that the SCN and CM could act as patient advocates, working together to reduce fragmentation across care phases and to minimise the misconceptions that may arise when information needs to be shared between professionals (Hudon et al, 2018).
In the ERAS model presented in this article, the CM integrates roles frequently assigned to the ERAS nurse and the discharge co-ordinator nurse, leading to a more cohesive approach to patient management and reducing the fragmentation of care (Kelly et al, 2019). In ERAS pathways, such integration empowers patients to feel more in control, address issues promptly, and learn to manage their condition effectively (Gustafsson et al, 2011). Additionally, educational pathways for patients with an ostomy have the potential to reduce complications, improve outcomes and enhance adherence to ERAS pathway components (Nizum et al, 2022).
However, having an ostomy, in particular an ileostomy, and the need for a patient to adapt quickly to living with a stoma, has been described as the Achilles heel of the ERAS pathways in colorectal surgery (Van Butsele et al, 2021) – patients with an ileostomy have high rates of hospital readmission related to dehydration/renal insufficiency (Messaris et al, 2012; Omar et al, 2023). A recent multicentre study describes this issue in Italy (Ferrara et al, 2024).
Since 2012, Mauriziano Hospital in Turin, Italy, has adopted the ERAS protocol for general and oncology surgery (Mineccia, 2020). Since 2019, the CM has overseen the co-ordination of the care pathway for complex patients, eg those undergoing hepatic, pancreatic, gastric or colorectal surgery. Compared with a control group, patients whose care was co-ordinated by the case management group had a significantly shorter hospital stay (9.64 days v 10.77), a shorter time span up to the point the patient was ready for discharge (0.60 days v 1.09), and patients showed greater autonomy in the activities of daily living (3.23 v 4.49) (Rizzo et al, 2021).
Historically, the length of stay for ERAS patients who do not require assistance at home with activities of daily living following discharge has been relatively short. Recent studies have highlighted the benefits of applying the ERAS protocol in cases of emergency surgery as well cases of elected procedures (Ahmed et al, 2024; Downey et al, 2024). However, when patients face changes in daily living such as loss of self-sufficiency and the presence of a stoma, length of stay increases and often necessitates the use of care services in the community, including nursing homes or home nursing care services. Furthermore, community SCNs are rare in Italy. In a previous study by the authors (Ariu et al, 2024), a significant percentage of patients with loss of self-sufficiency and an ostomy did not return home. This was not only due to the presence of the ostomy, but also because the patient had lost autonomy and had not received education on how to manage their stoma at home. Recent studies have indicated that there is a high incidence of missed nursing care for ostomy patients. Significant gaps in stoma care include patient education, mobilisation, nutrition, clinical monitoring, comprehensive discharge planning and follow-up. These omissions may contribute to the increased need for additional healthcare interventions for such patients post discharge (Valenti et al, 2024).
The collaboration between the SCN and the case manager (case management/stoma care CASTOMized project) aims to ensure careful planning of nursing activities, and support continuity and co-ordination of care. This partnership brings the two roles together at the patient's bedside, facilitating home discharge and reducing hospital readmissions.
Although other studies have examined the impact of having a nurse co-ordinating the process within an ERAS pathway (Jensen, 2021), this specific synergy has not yet been investigated and reported in the literature. The purpose of the study reported in this article is to describe the integration of roles in relation to the patient pathway within the ERAS protocol, with the aim of facilitating home discharge and reducing hospital readmissions.
Study design
This was a retrospective observational study.
Materials and methods
The study population included all consecutive patients who underwent major colorectal surgery with a stoma diversion, electively or in an emergency setting, in the Division of Oncological and General Surgery of Mauriziano Hospital in Turin between 1 January 2023 and 31 December 2023.
Patients with cognitive impairment and/or sensory impairment, even where this was temporary, and they required the assistance of a caregiver, were included.
Patients who were discharged to other healthcare facilities were excluded.
All patients, without exception, who underwent elective colorectal surgery, were treated under the ERAS protocol.
Intervention
The SCN and CM act synergically for elective patients, beginning with the prehospitalisation period. In counselling meetings lasting 45-60 minutes, they share information gathered in the preoperative period (20-30 days before surgery). In addition, the CM and SCN each have an in-person meeting with the patient and the family in which they outline a comprehensive perioperative course and how to manage the patient's care and wellbeing following surgery.
In this early phase, the CM proceeds with a preoperative nursing evaluation of a patient's mental capacity that may affect their ability to self-care, and undertakes one-to-one counselling to inform the patient of the specific perioperative path and ERAS protocol. These conversations help reduce a patient's preoperative anxiety and enhance adherence to and compliance with the pathway (Aasa et al, 2013; Hounsome et al, 2017; Ruiz Hernández et al, 2021). In this phase, post-surgical side-effects and consequences related to delirium, postoperative nausea and vomiting, and potential complications in the discharge process, as well as the possible need for venous access for postoperative hydration/parenteral nutrition, are evaluated.
Mineccia et al (2022) showed that the use of the stoma-therapeutic care pathway (STCP) facilitates preoperative patient education by the SCN, with a focus on nutrition, lifestyle, preoperative anxiety and providing instructions on the management of the stoma, taking into account the patient's experiences and expectations (Figure 1). Its aim is to support the patient's rapid adaptation to living with a stoma, and to reduce length of hospital stay (Forsmo et al, 2016; van Loon et al, 2020). Another STCP described in the literature was based on a best practice guideline developed to support patients on the ERAS pathway undergoing colorectal surgery in hospitals in Ontario, Canada (Miller et al, 2017). In this model, patients had autonomy in managing their stoma and took responsibility for their own role in the healing process.
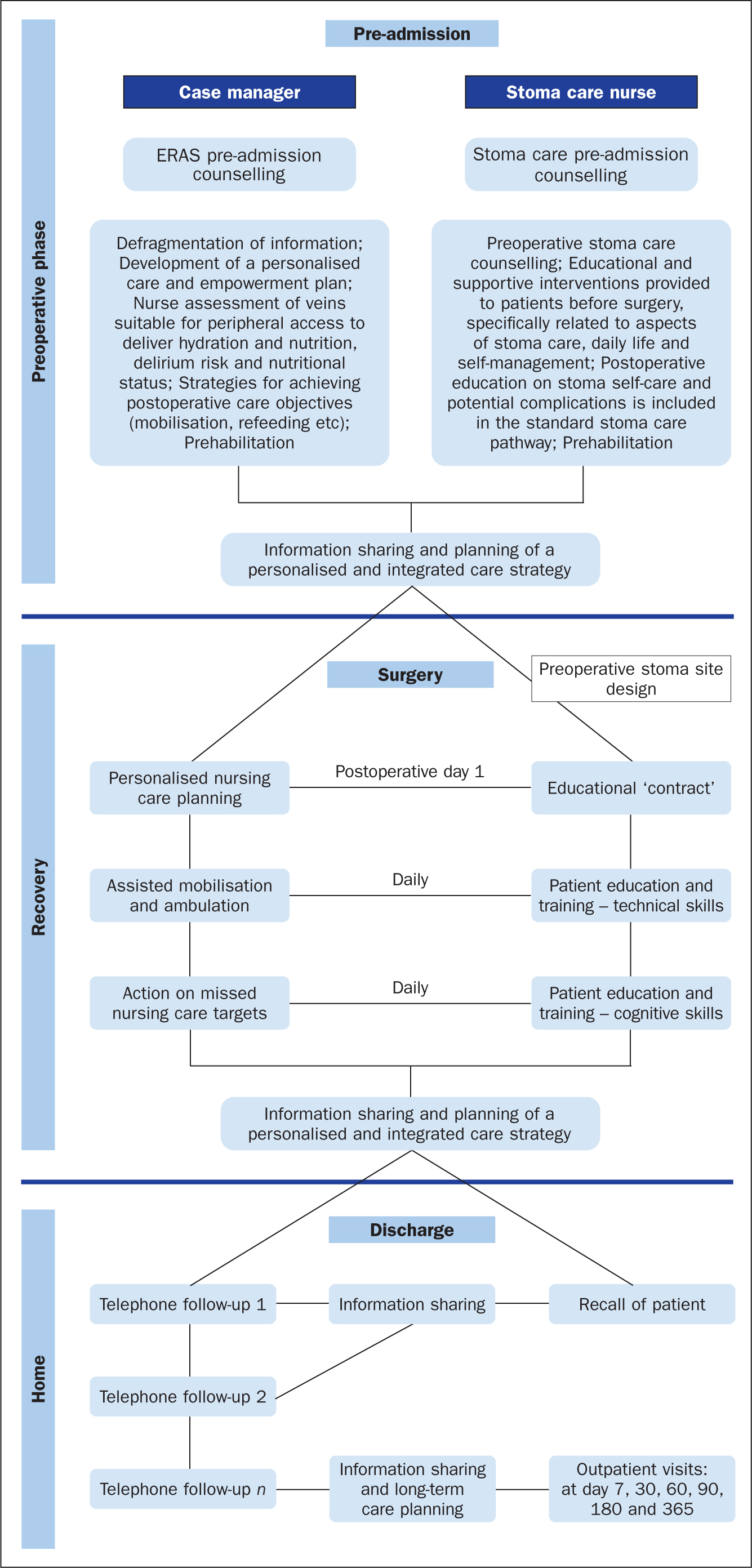
Preparation for the procedure pre-hospitalisation includes providing patient education and involving the individual in planning where to site the stoma; this is recorded in the clinical notes, along with the patient's demographic data. The prehabilitation interventions are supported by the SCN and CM, who outline the benefits of adequate physical activity and a healthy lifestyle, for example promoting smoking cessation and encouraging a reduction in alcohol intake.
To support the delivery of preoperative information, the use of educational tools such as booklets, audiovisual aids and communication techniques is tailored to meet the specific needs of each patient, and to clarify any doubts the patient has. Their level of understanding is subsequently assessed using the ‘Teach-back method’ (Ha Dinh et al, 2016).
The SCN and CM share the patient's demographic data, the results of any assessments and planned objectives via the patient's medical record with the other nurses and physicians involved in the patient's care.
During hospitalisation, the CM plays a crucial role not only in supervising standard care procedures, but also in enhancing specific interventions to optimise patient mobility and recovery. Additionally, the CM works to improve or maintain the patient's levels of autonomy in activities of daily living while ensuring adherence to ERAS pathway components.
Patients are assessed daily, and specific care interventions are planned strategically. Interventions encompass educational components, eg empowerment and health information, and are designed to enhance the patient's day-to-day functioning (such as walking and recovery of independence), as well as lifestyle choices that affect health, for example dietary habits and fluid intake. In addition, parameters such as weight and fluid balance are stringently monitored.
The STCP progresses through an educational ‘contract’ (a mutual agreement between the SCN and the patient that outlines educational goals and expectations) and involves regular consultations with the patient and/or caregiver to assess progress in meeting these objectives. The consultations, which take place in the patient's hospital room, also provide the opportunity to emphasise the importance of understanding potential changes in activities of daily living, relationships and sexual activity, as well as the need to adapt to new nutritional habits and bowel patterns. Both professionals continually discuss with the wider team meeting the patient's basic needs and their clinical progress.
On the day of discharge, the SCN assesses the patient's or caregiver's proficiency in using the stoma device, with a focus on identifying early problems. Following discharge, an integrated 30-day telephone follow-up is arranged between the SCN and CM and the patient and/or caregiver. The follow-up schedule includes standard telephone calls from the CM at 24 hours, and at 5 and 25 days after discharge, as well as recall of the patient to the SCN within 48–72 hours of discharge according to the CASTOMized protocol, and to provide information on the efficacy of the stoma and any complications (Gonella et al, 2019); however, the standard schedule can be adapted depending on clinical need. Any additional contacts with the patient are based on the needs identified during regular clinical assessments, with ongoing information and data sharing between the CM and the SCN.
During the telephone contacts, the CM elicits information from the patient to monitor signs and symptoms, paying specific attention to enteric output, diuresis, weight, water and food intake, and stoma-related complications. When necessary, the CM and SCN reinforce information regarding the administration of medications and their side-effects, summarising the treating physician's instructions using the teach-back method. The team assesses the patient's level of understanding and adherence to treatment, sharing any emerging issues with the ward surgeons, who have oversight of the ongoing assessments. If necessary, an outpatient or emergency department visit is organised.
The CASTOMized integrated process is illustrated in Figure 1.
Data collection
The patient data reviewed for this article were available from an institutional prospectively maintained database. The information reviewed included medical history, demographics, educational level, caregiver presence, diagnosis on admission, comorbidities, lifestyle habits, duration of hospitalisation, details of surgery, postoperative management, risk of readmission within 30 days, and remote interactions that occurred between the two professionals and the patient after discharge.
Length of stay was defined as the number of days from date of admission to date of discharge. Time to discharge was defined as the number of days between admission and the date of clinically possible discharge, as identified by the surgeons. These data are recorded in the patients' electronic medical records.
The database additionally contains information on adherence to the STCP and case management pathways (Figure 1), and ERAS protocol, as well as stoma-related complications, and whether the SCN was able to contact the patient for the scheduled follow-up telephone recalls. The nurse-related items in the ERAS protocol included counselling, preoperative carbohydrate loading, early mobilisation, early oral intake and symptom control.
Ethical considerations
Ethics committee approval was not required for this observational study. When patients were admitted they were asked to provide informed consent for data collection. The research data were collected by the co-investigators and stored in the hospital archive.
Data analysis
The statistical software package SPSSv27.0 was used by a professional not directly involved in the study for analysis with experience in biomedical statistics. The patient characteristics were evaluated using descriptive statistical procedures: continuous variables were summarised using median and minimum-maximum range, while discrete variables were analysed using absolute frequencies and percentages.
Results
Over the study period, 99 consecutive patients requiring a stoma were assigned to management using the CASTOMized integrated approach. The cohort was predominantly male (58.6%), with an average age of 62 years. The majority of patients (65.7%) had a cohabiting caregiver on discharge. The most common procedures performed were total proctocolectomy with ileo-pouch anastomosis, anterior rectal resection, in both cases with a temporary loop ileostomy, and total colectomy with end ileostomy, primarily for colorectal cancer (CRC) or inflammatory bowel disease (IBD). An ileostomy was created for 73.7% of patients, with 26.3% having a colostomy. The patients' demographic characteristics are detailed in Table 1.
| General characteristics | n (%) |
|---|---|
| Gender | |
| Female | 42 (42.4) |
| Male | 57 (58.6) |
| Age (mean-SD) | 62.23-18.50 |
| Presence of cohabiting caregiver | 65 (65.7) |
| Comorbidities | |
| Cardiovascular | 42 (42.4) |
| Diabetes | 8 (8.1) |
| Respiratory | 7 (7.1) |
| 2+ comorbidities | 12 (12.1) |
| Reason for treatment | |
| Colorectal cancer | 47 (47.5) |
| Inflammatory bowel disease | 41 (41.4) |
| Diverticulitis | 7 (7.7) |
| Other | 4 (4.4) |
| Surgery | |
| Total proctocolectomy and ileal pouch-anal anastomosis | 21 (21.21) |
| Low anterior resection | 18 (18.2) |
| Total colectomy | 18 (18.2) |
| Hartmann procedure | 12 (12.1) |
| Abdomino-perineal resection | 9 (9.1) |
| Stoma setup | 8 (8.1) |
| Left colectomy | 7 (7.1) |
| Ileocolic resection | 6 (6.1) |
| Other associated surgery | 11 (11.1) |
| Setting | |
| Elective surgery | 59 (59.6) |
| Elective surgery with neoadjuvant therapy | 17 (17.2) |
| Emergency surgery | 40 (40.4) |
| Ostomy type | |
| End ileostomy | 28 (28.3) |
| Loop ileostomy | 45 (45.3) |
| End colostomy | 20 (20.2) |
| Loop colostomy | 6 (6.1) |
Median hospital stay was 11 days, with an interquartile range of 9 days, and 40% of patients underwent an emergency procedure. A median difference of 0 days was observed between time ready to discharge and length of hospital stay. Complications occurred in 27% of cases during hospitalisation, most of which were low impact and resolved with medical or conservative treatment. Stoma-related complications occurred in 15% of patients, and 10% experienced mild peristomal skin complications (<2 on the SACS tool developed by Bosio et al (2006). High enteric output was recorded in 9% of patients (see Table 2).
| Total patients n=99 | Colostomy patients n=26 | Ileostomy patients n=73 | |
|---|---|---|---|
| Outcomes and clinical course: recovery to point of discharge | Median, days (IQR) | Median, days (IQR) | Median, days (IQR) |
| Length of stay (LOS) | 11 (9) | 11 (9.5) | 11 (9) |
| Time ready to discharge (TRD) | 11 (9) | 11 (10) | 11 (9) |
| Time difference between LOS and TRD | 0 (0) | 0 (0) | 0 (0) |
| SD (days) | SD (days) | SD (days) | |
| LOS | 12.9 | 5.7 | 14.7 |
| TRD | 12.9 | 5.8 | 14.6 |
There was an adherence rate exceeding 90% to both case management and stoma therapy pathways (see Table 3). Post discharge, nearly all patients were followed up remotely, but there was a decrease in adherence to telephone follow-ups over time, from 98% to 92%. Patients who did not respond to three remote contact attempts were considered non-adherent. Adherence to the ERAS protocol (namely, the items within the nurses' remit, such as mobilisation post-surgery, early refeeding and careful postoperative pain management) was 98%.
| Pathway Adherence | n patients (%) |
|---|---|
| Adherence to the ERAS pathway (nurse-led stoma management items) | 98 (98.98) |
| Adherence to the stoma care pathway | 95 (95.95) |
| Adherence to the case management pathway | 98 (98.98) |
| Recall adherence | 94 (94.94) |
| Case management follow-up call 1 adherence | 97 (97.97) |
| Case management follow-up call 2 adherence | 93 (93.93) |
| Case management follow-up call 3 adherence | 91 (91.91) |
Most patients were discharged to their own homes (90%), with only 5% requiring transfer to a nursing home, and 4% returned home with planned healthcare services support.
After discharge, 53% of patients reported a variety of symptoms or concerns. The most prevalent concerns among this subgroup related to fatigue (63%), changes in bowel habits (40%) and pain (17%), with 24% of patients experiencing more than one symptom. In all cases, remote care interventions were implemented.
Remote interventions were effective in 89% of cases (Table 4). These interventions primarily focused on diet (58%), resumption of self-sufficiency (27%), medication management – such as anti-diarrhoeal therapies for ileostomy patients or pain management as per discharge instructions (35%) – activities of daily living (16%), including returning to work, sports or doing household tasks, and managing the peristomal site (16%).
| Outcomes and clinical course: after discharge | n (%) |
|---|---|
| Readmission rate | 13 (13.1) |
| Surgical complications | 7 (7.7) |
| Abdominal subocclusion | 3 (3.0) |
| Abdominal abscess | 2 (2.0) |
| Surgical wound infections | 2 (2.0) |
| Medical complications | 3 (3.0) |
| Fatigue and loss of appetite | 1 (1.0) |
| Fever | 1 (1.0) |
| Lung infection | 1 (1.0) |
| Renal failure/dehydration | 3 (3.0) |
| Remote care interventions | 53 (53.5) |
| Decisive remote intervention | 47 (88.7 *) |
Thirteen per cent of patients were readmitted, with 7.7% of cases due to sudden surgical complications without prior symptoms, and 6% following a nurse-led report (from the CM or SCN). In the immediate post-discharge period, 15% of patients had a high-output stoma (>1000 ml/day); however, only 3% of this group required readmission. The SCN and CM implemented regular monitoring, electrolyte replacement therapy, dietary adjustments, and provided patient education for the remaining 97% of these high-output patients, which helped prevent readmission (Table 4).
Discussion
The formation of an ostomy as part of colorectal surgery has both benefits and drawbacks for the patient (Vonk-Klaassen et al, 2016). It is often the case that patients who are ready for discharge have their hospital stay prolonged due to problems with organising independent stoma care in their home – which also results in increased healthcare costs. However, if the number of patients who do not require home nursing services being discharged to their own homes can be increased this will free up the availability of home nursing care services for other patients. The importance of providing stoma education for patients having colorectal surgery is another well-recognised issue (Chaudhri et al, 2005). These are all well-recognised issues in stoma surgery and management.
Tailored educational programmes have been proven to be effective in improving the knowledge and self-care of patients with an ostomy (Sacks et al, 2015; van Pelt et al, 2024). A study by van Loon et al (2020) demonstrated that a ‘four-day in-hospital educational stoma pathway’ for ostomy patients increased their independence and reduced reliance on home nursing care services. Patients received comprehensive stoma care education, promoting independence through supervised practice, caregiver involvement and dietary counselling, from the time of admission to postoperative day 4, with daily visits from the SCN. The study found that, after discharge, the proportion of patients requiring daily home nursing services decreased from 80% to 50%, while the proportion of those able to manage their stoma independently rose from 5% to 27% (van Loon et al, 2020).
To the authors' knowledge, the study reported in this article is the first to explore the collaboration between an SCN and a CM within colorectal surgery paths involving ostomy placement.
The authors focused on restoring patients' independence and self-care, enabling them to return home to manage independently. In addition to the involvement of the SCN and CM, collaboration with other professionals, such as dietitians and physiotherapists, contributed to fewer home service interventions and nursing home admissions. The authors' educational initiatives targeted both patients and caregivers, which was likely to have contributed to the reduced use of home nursing services. Before the implementation of the CASTOMized model, the SCN had been the sole professional responsible for engaging caregivers with regard to the patient's post-discharge needs, with interventions focused principally on stoma management.
The primary goal of this project was to develop and design a home discharge plan to enable the patient to live independently, given the undeniable advantage of this in terms of quality of life compared with discharge with input from home nursing care services or discharge to nursing homes. The time necessary to put these services in place can lead to an extended length of hospital stay or the risk of hospital readmission post discharge. These issues were evident in the authors' sample of colostomy patients and correlated with the type of surgical procedure each had undergone, the major postoperative complications experienced, and the patient's age. In this study, the high number of patients treated as emergency cases and the number who had to undergo additional surgeries contributed to a longer length of stay compared with that reported by other studies; median length of stay was 11 days, which compared with 6 days reported by Catarci et al (2022) and 5 days by Mangone et al (2024). In this study, the length of stay was 11 days, irrespective of stoma type (Table 2); this is in contrast to a reported trend for patients who have had a colostomy or ileostomy experiencing different complications and therefore requiring different length of hospitalisation (Malik et al, 2018).
Further confirmation of the effectiveness of the collaborative SCN/CM approach is illustrated by the fact that difference between time to discharge and length of stay was negligible (Table 2) compared with that reported by previous studies (Celio et al, 2019). This indicates that the recovery planning approach used in the authors' study is effective, with the home discharge rate achieving 90%. In addition, the readmission rate remained significantly lower than that reported by other studies (Damle et al, 2016). The implementation of the authors' integrated pathway demonstrated better patient adherence to follow-up and included daily scheduled telephone calls to address any post-surgical symptoms indicative of complications, such as lack of appetite, reduced hydration or high ostomy output. This prompt identification of potential problems was facilitated by educating patients and caregivers about potential warning signs, which enabled effective symptom management. For instance, patients received guidance with regard to dietary adjustments, fluid intake and the use of thickening supplements, or were prescribed loperamide to manage high ostomy output (Gonella et al, 2019).
The findings of the present study also highlight that, although the risk of dehydration remains significant at home, readmission rates were lower than reported by previous studies due to co-ordinated follow-up by the care team. The literature describes dehydration related to ostomy formation, often an ileostomy, as having a significant impact on patients' quality of life and costs, with incidence rates ranging between 3% and 40% (Messaris et al, 2012; Vogel et al, 2022; Omar et al, 2023).
Symptoms such as fatigue, changes in bowel habit, pain and reduced appetite are common following colorectal surgery, but have shown a decreasing trend in the authors' hospital with the introduction of telephone follow-up, as reported previously (Ariu et al, 2024). The above symptoms, while typical in postoperative recovery, are not always easily self-managed by patients. Consequently, many require telephone support, emphasising the need to provide them with information and support on the self-management of symptoms (Husebø et al, 2023).
High adherence to the STCP also accounts for other positive outcomes, such as the reduced incidence of peristomal skin complications compared with that reported elsewhere (D'Ambrosio et al, 2022), although this is a complication prevalent among colostomy patients (Maglio et al, 2021). The follow-up outcomes, in terms of adherence, can be attributed to the authors' consistent presence at the patient's bedside, which enabled individual patient needs to be addressed throughout the entire surgical pathway. This implementation of and adherence to the pathway fosters the establishment of trust between the health professionals, patients and their families, and supports the achievement of agreed educational objectives.
Conclusion
This study highlights the significant benefits gained by entrusting advanced practice nurses with the implementation of integrated management of care pathways. The collaborative approach to stoma management between the SCN and CM has been shown to be effective in addressing patient adherence to clinical pathways and enhancing the patient's stoma management and wellbeing following discharge to their own home.
Despite there being a risk of dehydration for patients discharged home, the authors' co-ordinated follow-up programme has reduced readmission rates, highlighting the effectiveness of the integrated care model.
One key finding is the importance of implementing an educational programme to enhance patient knowledge and stoma self-management.
Looking forward, it is essential to continue refining the integrated pathway and expanding its application to other surgical areas. Future research should focus on understanding the long-term outcomes and cost-effectiveness of the approach described in this article, as well as exploring ways to further enhance patient education and support.


