Urinalysis, electrocardiography electrode placement, peripheral venous canula choice, blood specimen bottle choice, cardiac monitoring electrode placement and central line care/management, to name but a few procedures, all share commonalities other than being clinical nursing skills. They all require a degree of colour perception—but what if someone is colour blind?
Although often described as colour blindness, this is the wrong term for the condition. The broader definition is colour vision deficiency (CVD), of which there are several variants (Table 1). In fact, it is rare to be completely ‘blind’ to colour, a condition that is known as monochromacy or achromatopsia.
Table 1. Types of colour vision deficiency
| Type | Effects | Impact on nurses with CVD |
|---|---|---|
| Deuteranomaly | The inability to differentiate between shades of green (deuteranomaly) and red (protanomaly) | Potential problems include:
|
| Protanopia and deuteranopia | More severe versions of deuteranomaly and protanomaly | |
| Tritanopia | The inability to differentiate between shades of blues and yellows | |
| Trichromacy | The inability to differentiate between the three primary colours of red, green and blue | |
| Monochromacy or achromatopsia | The inability to differentiate between any shades of colours, seeing black and white only |
CVD is normally inherited by children from their parents through a genetic fault, which manifests as cells missing from the cones in the eyes, or the cones functioning incorrectly (NHS website, 2019). It is likely to be significantly underdiagnosed and is a condition that many people do not understand, or realise what it is and how it affects those who have it, and there also is little awareness of its prevalence.
The National Eye Institute (NEI) describes ‘colour blindness’ as the ‘trouble telling the difference between colours’ (NEI, 2019) and highlights that the condition usually runs in families. It has no cure, but most people have no issues in undertaking everyday activities and adapt well to living with CVD.
In an article aimed at school nurses, Albany-Ward and Sobande (2015) suggested that ‘it is caused by faulty gene sequencing in the DNA of the X chromosome’, adding that ‘colour is an important tool, but for colour blind students it can be a nightmare—undermining confidence, encouraging basic errors, making them slower to follow instructions and causing frustration and even anger’.
But what are the effects of CVD in adulthood and, specifically, people with careers in health care? Can the condition impact a nurse's ability to carry out their role independently and autonomously? Articles in medical and dentistry journals have focused on the actual or potential impact of colour blindness on students in these fields (Spalding, 2004; Spalding et al, 2010; Goh et al, 2014; Raynor et al, 2019). These articles consider some of the tasks that might prove difficult, and these can be translated to nursing, including procedures such as electrode placement and central line management as noted earlier.
Other potential problems include being able to identify haematuria in a patient's urine or melaena in stool (Reiss et al, 2001). A study by Katmawi-Sabbagh et al (2009) found that patients with CVD presented with later stages of bladder cancer than those without CVD, which, the authors suggested, was linked to patients' difficulties with colour perception. Although the study investigated colour perception among patients, it could be surmised that nurses with CVD could also be missing these signs and symptoms.
GP, writer, editor, podcaster and educator Euan Lawson is a health professional with CVD. In two podcasts he talks about his experiences of CVD as a doctor, for example, the challenges of identifying colours on urine dipsticks. He was able to recognise the tonal differences of some colours if the dipstick was positioned a certain way rather than relying on the actual colours. However, if the results were likely to show as pink, he would rely on peers or even patients to interpret the results for him. He points out that certain career paths, for example in surgery, would have caused problems in terms of recognising the colour of organs inside a body cavity. In another podcast he discusses the issues with campaigner Kathryn Albany-Ward, who founded a website to raise awareness about ‘colour blindness’ (https://www.colourblindawareness.org). The website is a good starting point for understanding the issues surrounding colour blindness and is a resource recommended by the NHS for both patients and health professionals.
Prevalence among nurses
In 2020, 724 516 nurses, midwives and nursing associates were registered with the Nursing and Midwifery Council (NMC), of whom 10.7% identified as male and 89.3% as female (NMC, 2020). The prevalence of CVD in the UK is estimated to be 1 in every 12 males and 1 in 200 females (NEI, 2019; NHS website, 2019), which would mean that around 9695 of NMC registrants are likely to have the condition.
Although CVD is not acknowledged as a disability, the UK's Government Equalities Office recommends that schools, businesses and employers should treat people with the condition as they would treat people with a registered disability (Colour Blind Awareness, 2021).
Thankfully, many items of equipment used in nursing practice, such as electrocardiography electrodes, are numbered as well as colour coded (Figure 1), making them more appropriate for practitioners with CVD. However, it is impossible to include such fail-safes in, for example, identifying haematuria or melaena, or interpreting urinalysis. In the absence of a device to support identification of test results, practitioners may need to call on their colleagues to help with such interpretations to ensure that a patient's vital signs are correctly recorded and symptoms are not missed.
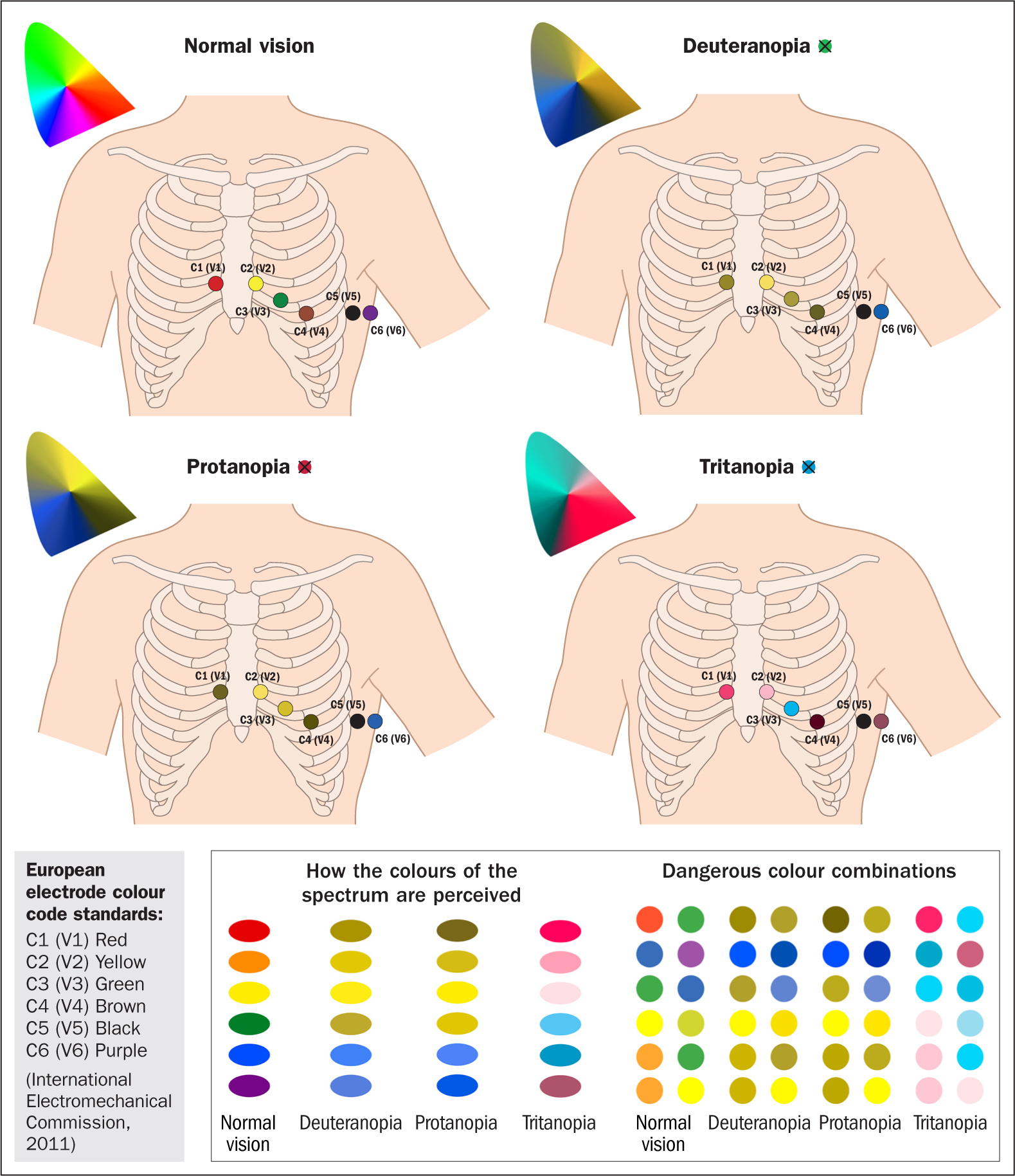 Figure 1. Approximate representation of how colours are perceived by people with colour vision deficiency compared with those with normal vision in the context of ECG monitoring
Figure 1. Approximate representation of how colours are perceived by people with colour vision deficiency compared with those with normal vision in the context of ECG monitoring
Conclusion
It is important to consider how practitioners with CVD may be affected when carrying out nursing duties. Aside from clear practicalities, it is important to consider how having CVD could undermine an individual's confidence, lead to basic errors, and make the person slower to follow instructions, causing frustration and even anger. This is an area that needs more research, particularly due to the underdiagnosis of CVD and the lack of information about its prevalence among nurses. It is important to raise awareness about CVD and how it affects nurses in order to increase understanding among the profession and to encourage universities, colleagues and employing organisations to put in place systems to support nurses with CVD.
LEARNING OUTCOMES
- 1 in 12 men and 1 in 200 women have colour vision deficiency (CVD). Actual ‘colour blindness’ or monochromacy/achromatopsia is very rare
- Nurses with CVD might need peer and employer support to prevent harm and help avoid mistakes in practice
- There could be over 9500 health professionals with CVD on the Nursing and Midwifery Council register
- CVD is not a registered disability, but employers, universities and schools, for example, should treat those with CVD as they would a person with a registered disability


