A professional practice model (PPM) provides ‘the overarching conceptual framework for nurses, nursing care, and interprofessional patient care’ (American Nurses Credentialing Centre (ANCC), 2014), and can be described as a schematic representation of a profession (Murphy, 2011).
The ANCC runs the Magnet scheme, which recognises nursing excellence, and publishes the Magnet manual that describes all the relevant components that organisations are required to work on in order to achieve Magnet designation (Box 1). The latest Magnet manual (ANCC, 2019) asks organisations to provide examples of improved outcomes associated with a change brought about by clinical nurses in alignment with a PPM.
Many organisations develop PPMs as part of their Magnet journey. NHS Grampian had been exploring the Magnet scheme and decided to adopt some of its underlying principles. As part of this, the development of a PPM was a sensible step to take. The health board began exploring Magnet in early 2016 and the author's role was to gather information, make contact with experts and commence working on relevant principles. An academic colleague had visited Magnet hospitals as part of a Florence Nightingale Foundation Leadership Scholarship and it was decided that the author, a senior nursing clinical lead, should apply for a scholarship to enable her to visit Magnet designated hospitals as part of information gathering.
The application for a Florence Nightingale Travel Scholarship was successful and preparatory the research focused on visiting three Magnet-accredited hospitals in Australia—the Princess Royal Alexandra Hospital in Brisbane, the Sir Charles Gairdner Hospital in Perth and the St Vincent's Hospital in Sydney—talking with organisations in Australia that had decided not to work towards Magnet status, and also to participate in a UK interest group, NAME UK (a group of organisations interested in Magnet). For Australia, contact was initially made with one of the Magnet programme directors, who introduced the author to the programme directors of the other two hospitals.
Methodology
Colleagues in Australia shared details of their PPM development process, to support NHS Grampian's desire to implement a PPM. A number of colleagues across the UK also shared their processes around PPM development, and examples of PPMs were obtained by conducting a general search online.
A short-life working group was established using a shared governance approach (Taylor, 2016), whereby staff from any area of the organisation and from any level of seniority could volunteer to participate. Slatyer (2015) noted that using the concept of shared governance as a basis for a PPM was a ‘recurring theme’ in literature on PPM development. The approach used by Australian colleagues was replicated and illustrated in Figure 1. Staff across the nursing, midwifery and allied health professions (NMAHPs) teams within NHS Grampian hospitals were invited to volunteer.
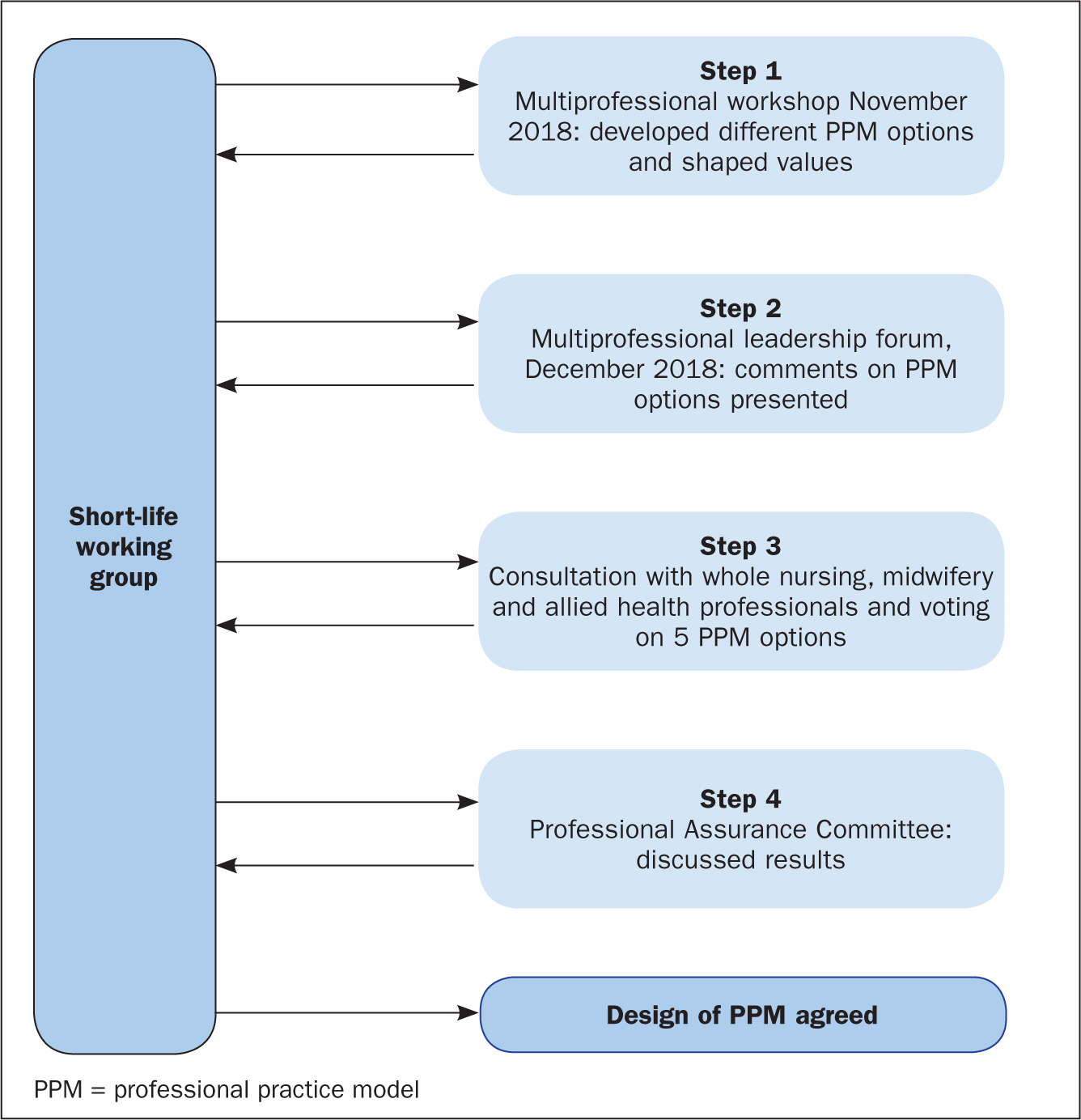
A cyclical process of development was decided upon, with the short-life working group being the spine overseeing the entire process. A shared governance approach ensured that staff were involved in decision-making about the design and process of developing the model.
Methodologies from the Australian hospitals and NAME UK colleagues confirmed that the development of a PPM should begin with staff workshops, which enable all levels and types of staff to participate in exploring a shared professional vision and values, and the core components that would make up a PPM (Small and Small, 2011). Box 2 provides a summary of the development process.
| September 2016 | Short-life working group set up |
| November 2016 | Workshop developed five options |
| December 2016 | Professional Leadership Forum considered and refined the five options |
| Jan-March 2017 | Nurses, midwifes and allied health professionals voted on the options |
| May 2017 | Results considered by the senior nursing, midwifery and allied health professions (NMAHP) leads |
| June 2017 | Presented work at quality event (an annual NHS Grampian quality and safety conference |
| October 2017 | Model finalised and distributed, presented at Celebrating Excellence Day on 1 November (These are held three times a year, and any member of the NMAHP staff can present their work orally or via a poster, and they are open to any members of staff to attend. Certificates are awarded at this event.) |
| November 2017 | Commenced distribution of leaflets and posters promoting the model to all NMAHP staff across the health board |
| April 2018 | Communications design Robert Gordon University contacted and project initiated |
The short-life working group designed an initial workshop, testing some of the activities in advance themselves. The subsequent organisation of the workshop took a shared governance approach, with invitations open to any members of staff. About 60 staff from across all professional groups volunteered to take part in the workshop, which included exercises to comment on how relevant the organisational vision and values were to them, to identify more specific professional values and to consider what a PPM might look like. The use of organisational values as the basis for a PPM are supported by the findings of Slatyer et al (2015), who stated that ‘the majority of models also incorporated organisational core values’. Five PPM options emerged from the development workshop, which were approved by the senior NMAHP group. The author contacted graphic design colleagues in the Corporate Graphics Department at NHS Grampian, who subsequently turned the hand-drawn proposals into formal designs.
PPMs are traditionally developed to represent the nursing workforce. Magnet component principles were being explored across the NMAHP groups, so the PPM aimed to represent the entire NMAHP community of the health board. Differences in professional views emerged through meetings, discussions and emails from staff: for example, the term ‘caring’ was thought to be associated more with nursing and the term ‘enabling’ with allied health professionals. Eventually, the short-life working group was able to agree final versions of the five PPM options that suited all professional groups.
The next stage involved sending the five options out for consultation with the 6500-strong NMAHP workforce with explanation of a PPM, and asking them to vote on their favoured option. Support with designing the survey was provided by the Clinical Effectiveness Team and about 1000 responses were obtained. The results were analysed and fed back to the committee of senior NMAHP leads and the short-life working group. The final, confirmed option was then produced in print format with the assistance of medical illustrations colleagues at the University of Aberdeen.
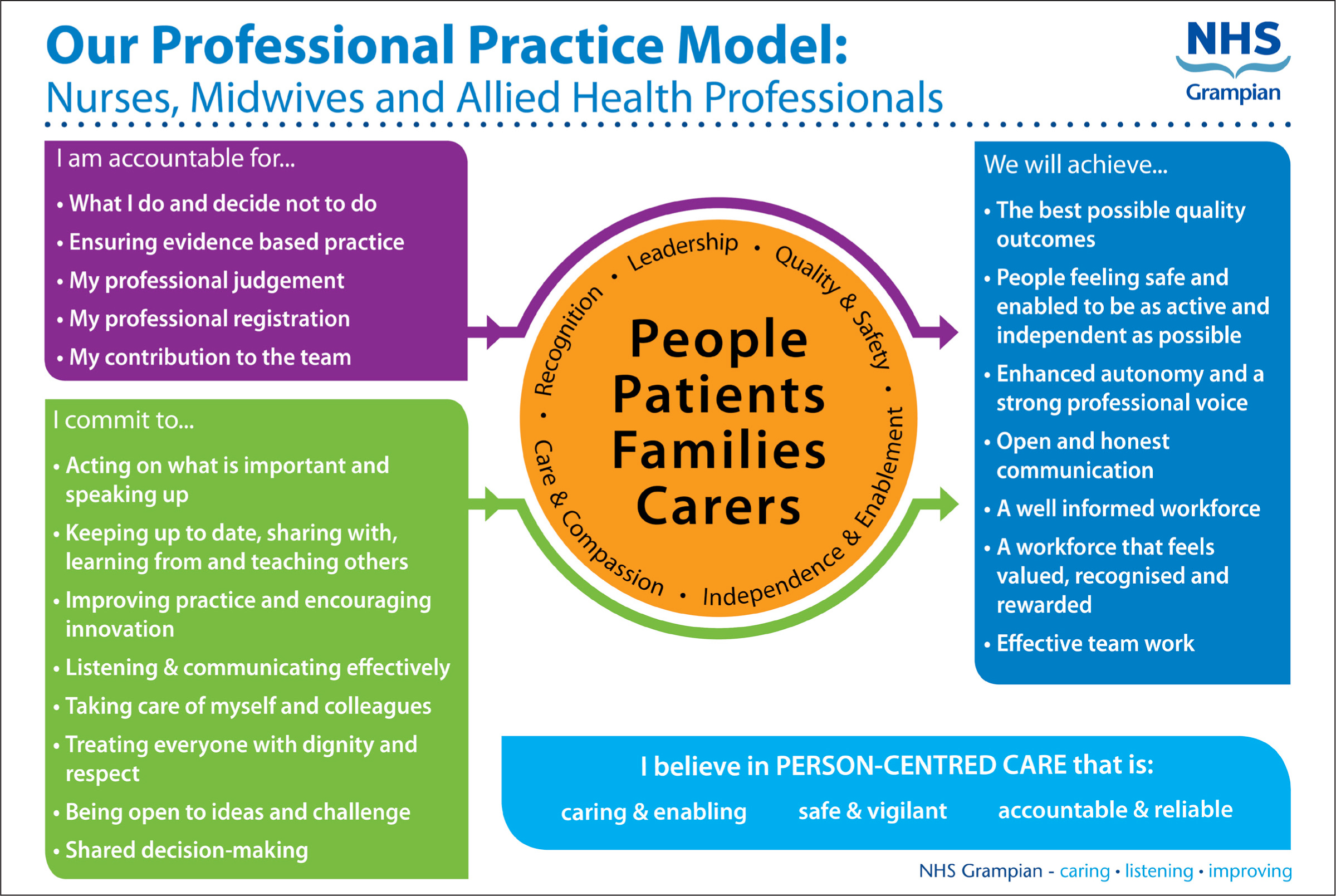
Part of the development process involved gaining suggestions about the production format for distributing the model, along with suggested uses of the PPM. Information on the uses of the model was obtained from one of the NAME UK organisations. To date, the NHS Grampian graphics team has produced the final PPM in a variety of formats, which have been distributed across the health board by the senior NMAHP team: for example, an A5-size diary, which is used mainly by staff in primary care, and A4 and A5 versions for display on noticeboards. Pens and sticky notes with the PPM logo (consisting of the orange circle from the centre of the PPM model, Figure 2) have been produced and the logo design adapted for use on smaller items. The aim was to produce a simple, one-page document that would contain everything staff needed to become familiar with the model and its uses, so print versions had the PPM (Figure 2) on one side with it uses listed on the reverse (Box 3).
| It could be incorporated or applied in: |
|
As staff started to use the model, requests came for additional adaptations in display, such as versions with blank boxes underneath to encourage staff to write what the PPM means to them or how they can relate to an aspect of the PPM. Early on, it was recognised that, because the NHS Grampian practice education team for NMAHPs work closely with direct care staff, it could assist with implementing the model. The author was told of different ways the PPM was being used with staff, eg the practice education team was using it in conversations with staff and within education-specific workshops. The PPM was not just stuck on a wall but was being used within the content of work.
Results and progress
The initial work conducted in the first workshop identified that what staff wanted was:
These elements were then incorporated within the PPM or made part of the developmental process.
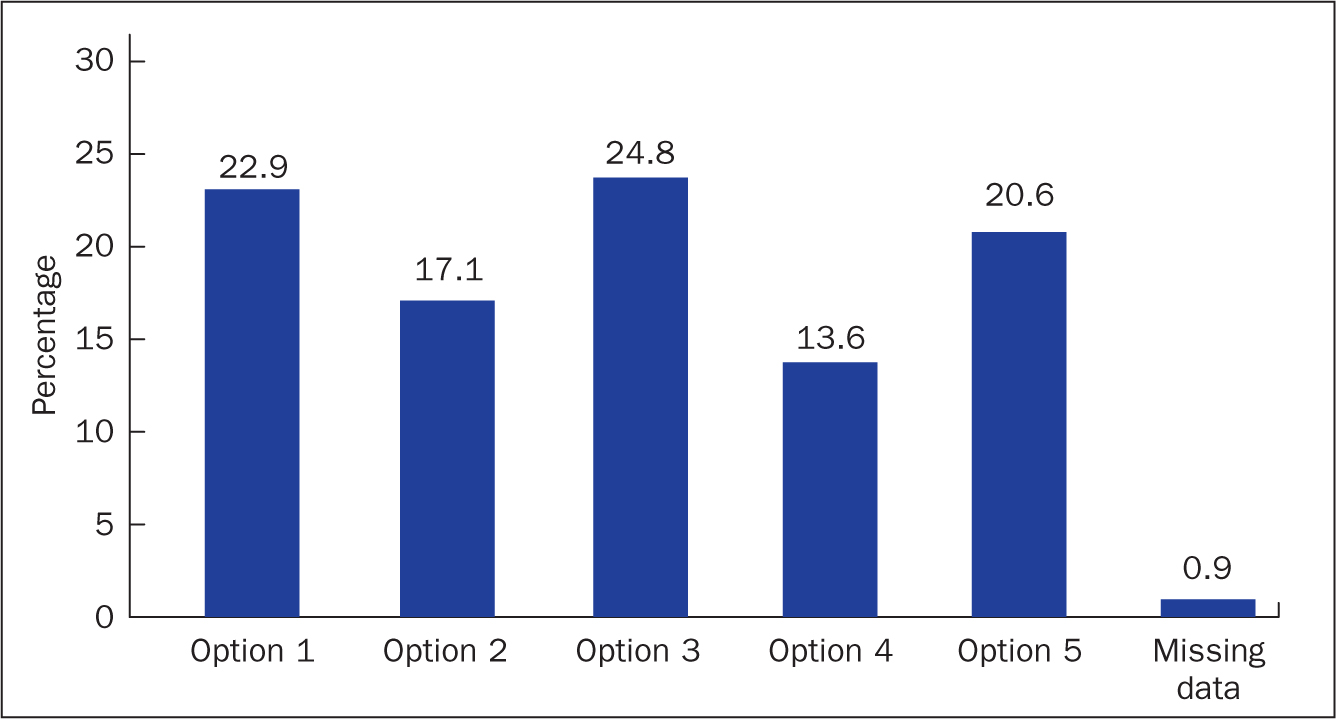
The survey voting on the five PPM options showed that most of the staff who had participated were nurses. This was not unexpected given the high percentage of this professional group in the organisation (Table 1). The results also showed that there was no overall preference for a particular model. Figure 3 shows that the differences were small: there was no clear winner, although model 3 gained the highest number of votes.
| Staff group | Number | % |
|---|---|---|
| Nurse | 529 | 58.9 |
| Midwife | 47 | 5.2 |
| Allied health professional | 267 | 29.7 |
| Other | 45 | 5.0 |
| Missing data | 10 | 1.1 |
The results shown in Figure 4 indicate the overall preferred options by professional grouping:
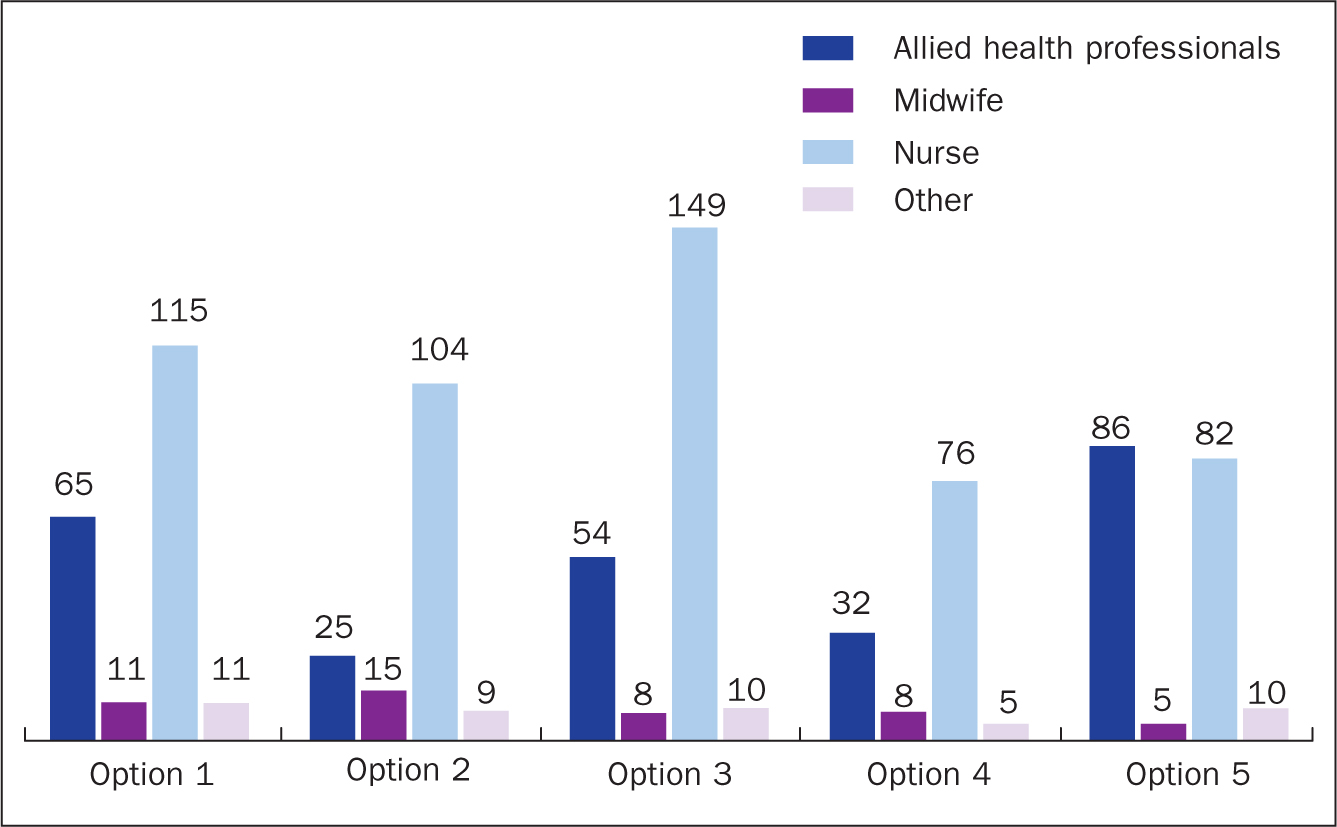
The short-life working group considered the results and then applied, to the option that gained the highest vote, a set of criteria derived from a combination of the Magnet standards, journal articles, the PPM development process and the professional codes of conduct in use at the Princes Royal Alexandra Hospital in Brisbane. Following this process, option 3 was designated as fit for purpose. The deciding factor was the fact that it had gained the highest percentage vote (24.8%). However, one senior staff member commented: ‘It's more important how we implement it.’ This version was sent to the NHS Grampian Corporate Graphics Department for further design work.
The selected option (Figure 2) shows that the focus is on people, patients, families and carers, with the terms ‘leadership’, ‘quality and ‘safety’, ‘independence and enablement’, ‘care and compassion and recognition’ represented around the outside of the central circle. The three boxes around the circle represent individual commitment, and individual and team accountability, for example:
‘A workforce that feels valued, recognised and rewarded’. Staff really welcomed having a visual representation of the links between individual staff accountability and what could be achieved collectively. Leaders also welcomed the explicit description of accountability that applied in a range of settings.
Considerable progress has since been made in implementing the PPM, which is positioned at the core of professional practice. The model has been incorporated widely, including:
Communication design students' work
The idea of working with university design teaching departments came from the recognition that NMAHP staff are educated for their clinical roles, but they are not experts in branding. The idea to involve students arose after the author saw another health board's presentation on collaborating with a design company and an awareness that organisations could approach universities for student placements.
The health board's graphic design department is very busy and it was thought that students from Robert Gordon University might provide fresh eyes. A proposal was submitted to the university's communication design course leader and two students expressed an interest in working on ways to promote the PPM with staff. The students met with the clinical teams to learn about their views on the PPM. They also used Facebook to elicit information from staff.
The students took their brief to be ‘To explore the development of communication tools, materials and methods for the dissemination and implementation of the model across the whole NHS Grampian NMAHP workforce’.
After meeting with the staff the students focused on three issues:
Empowerment
The students suggested that the NHS Grampian senior NMAHP leads should think of staff as heroes and develop powerful images to represent this concept. The inspiration was the Channel 4's promotional campaign for its 2012 Paralympics coverage, entitled Meet the Superhumans. The students later reflected that they wanted to ‘create an impression of staff being superhuman … because, after all, the amount of amazing work they do, it's time we start recognising it’. They suggested that the NMAHP senior team used the same concept to portray staff, moving away from the nurse in apron to a more powerful image of staff standing proudly in photos.
Personalisation
The students invited staff to write what was professionally important to them. They also invited them to write on a card what the PPM meant to them, and then take photographs of themselves holding the card. The idea was that writing down and taking a photo would be an interactive process that would personalise the model, prompting staff to think about the PPM and how its components relates to them, rather than being simply another poster on the wall.
NHS Grampian had used this kind of approach before, so this idea was appropriate for further exploration.
Promotion
This involved the use of branding via social media, with the idea of using the hashtag #weare, which could be used in photos, in banners to use at events and in promotional materials. Staff also used the following extended hashtags:
The final recommendation from the students involved some practical applications, such as Model Mondays, where a different weekly theme or activity could be used to promote the PPM. Although this was considered a worthwhile idea, it would have required considerable resources so suggestions for more practical but less frequent activities, or those requiring a longer time frame, were considered instead. This included, for example, organising monthly cake and coffee events and asking staff to dress up as superheroes at events and promotions. In addition, there was a suggestion to run a 6-month campaign featuring a different part of the PPM each month, eg ‘commitment month’. Promotional materials could be produced alongside to support the campaign and to promote ‘#weare’.
The students' recommendations were well received by the NMAHP lead team. There was acknowledgement that the students had come up with some new publicity angles. For example, the author and a colleague started using the hashtag #weare immediately, including it at the next NHS Grampian Celebrating Excellence event using the hashtag #wearecelebratingexcellence (Box 2).
The students reflected that they had found the work challenging and inspiring. They had wanted to create something that was ‘visual and empowering, a campaign that drives change’.
The senior NMAHP lead team concluded that the idea of involving nurse leaders in creating campaigns should be embraced, and their ideas could be supported by graphic design and communications colleagues, who have the skills to transform ideas into eye-catching designs. Branding is an important part of developing campaigns to support initiatives and strategic directions. The potential of working with other university departments, such as marketing students, to assist NHS Grampian with branding and spreading information, has also been welcome.
Evaluation of the development process
Following the design and selection of our PPM option, however, the author wanted reassurance around the methodology used to develop the content. When the author was in Australia, an article on the development of PPMs reporting a review of the relevant literature, was shared by Professor Susan Slatyer (2015), the lead author of the work. According to Slatyer et al (2015), the essential elements of a PPM include (also see Table 2):
| Literature review core components | Process used and content of a professional practice model (PPM) |
|---|---|
| Leadership |
|
| Nurses' independent and collaborative practice | Found in: |
| Environment | Taking care of myself and colleagues |
| Nurse development and reward |
|
| Research/innovation | The model promotes accountability around ensuring evidence-based practice, a commitment to improving practice and encouraging innovation, and keeping up to date |
| Patient outcomes |
|
| Shared governance | Included in the ‘I commit to …’ shared decision-making |
| Caring |
|
| Relationships | Features in the concepts of person-centred care |
| Magnet | Includes many elements of the Magnet concept, eg recognition, shared governance, best outcomes, people feeling safe, strong professional voice, autonomy, innovation, evidence-based practice etc |
Table 2 sets out the author's evaluation of the PPM developed at NHS Grampian against Slatyer et al's (2017) core components. Although Slatyer et al's work was a retrospective analysis, it was considered a useful exercise to check that the selected PPM measured well against the core components identified by Slatyer et al (2016) in their literature review. The process reassured the senior NMAHP lead team that the PPM developed was fit for purpose because it covered all of the core concepts suggested by Slatyer et al. However, the evaluation of the NHS Grampian PPM did reveal that the model was light on environmental aspects, which is something that can be strengthened at implementation stage and also taken into account at the review stage.
Conclusion
This article has looked at the process undertaken by one health board in the North East of Scotland to develop a PPM. A professional practice model is one of the requirements for attaining Magnet designation, a concept that NHS Grampian has explored with the decision to implement some of the principles, as outlined in the Magnet Application Manual (ANCC, 2014).
The author was supported by a Florence Nightingale Foundation scholarship to visit Magnet hospitals and attend UK-based Magnet-themed meetings. The areas visited shared their approaches to PPM development, which assisted the author in the development of a process for the health board where she works.
The article has discussed the shared governance approach undertaken, which involved a short-life working group made up of volunteer staff overseeing the PPM development process. A range of workshops were held, involving staff from across NMAHP teams, leading to the design of 5 PPM options. These alternatives were then presented to the whole NMAHP workforce to seek their views on the preferred model, following which a PPM was chosen, and then refined with the help of NHS Grampian Corporate Graphics Department.
The PPM has now been used in a variety of ways, ranging from its incorporation in the new NMAHP strategy to its use on conference posters, promotional material and recruitment flyers. A range of other approaches were suggested by two communication design students who were involved, and their suggestions are now being implemented.
The article has also presented an assessment the development process against findings from a literature review on the development of PPMs. This process reassured NHS Grampian that the PPM was fit for purpose, although it revealed that the model was light on environmental aspects. The results of this assessment will be considered again when the PPM is reviewed in a few years' time.

