Evidence-based practice (EBP) was first mentioned in the literature by Muir-Gray, who defined EBP as ‘an approach to decision-making in which the clinician uses the best available evidence in consultation with the patient to decide upon the option which suits the patient best’ (1997:97). Since this initial definition was set out in 1997, EBP has gained prominence as the gold standard for the delivery of safe and effective health care.
There are several models for implementing EBP. Examples include:
- Rosswurm and Larrabee's (1999) model
- The Iowa model (Titler et al, 2001)
- Collaborative research utilisation model (Dufault, 2004); DiCenso et al's (2005) model
- Greenhalgh et al's (2005) model
- Johns Hopkins Nursing model (Newhouse et al, 2005)
- Melnyk et al's (2010) model.
Although a comprehensive review of these models is beyond the scope of this article, a brief assessment reveals some commonalities among them. These include a) asking or selecting a practice question, b) searching for the best evidence, c) critically appraising and applying the evidence, d) evaluating the outcome(s) of patient care delivery, and e) disseminating the outcome(s).
Regardless of the benefits of EBP, and the existence of multiple EBP models intended to facilitate the application of evidence into practice, health professionals, including nurses, continue to struggle to implement it effectively (Ubbink et al, 2013). Critics of EBP have questioned its validity (Rubin, 2007; Nevo and Slonim-Nevo, 2011); the best practice and setting to support its use (Nutley et al, 2009); its failure to address the complexity of health and health care, as well as the patient's context (Muir-Gray, 1997; Reed et al, 2019), and its mechanistic approach (Epstein, 2009; Jerkert, 2015). Some of these criticisms are outlined below.
For example, previous studies have reported the barriers health professionals face to successfully implement EBP. Ubbink et al (2013) conducted a systematic review to determine nurses' and doctors' views on knowledge, attitudes, skills, barriers, and behaviour required to implement EBP. The review included 31 studies from 17 countries: eight from North America and 11 from Europe. The results revealed that organisational and individual barriers prevent uptake of EBP among nurses and doctors. These barriers included the lack of material and human resources, and lack of support from managers and leaders; individual barriers included knowledge deficit regarding EBP, time and workload (Ubbink et al, 2013). Researchers such as Hitch and Nicola-Richmond (2017) and Warren et al (2016) found similar barriers to implementing EBP reported by health professionals.
Effective and consistent implementation of EBP in healthcare settings depends on complex interdependent factors, such as the characteristics of an organisation (eg the internal and external healthcare environment, and organisational structures and values); the EBP intervention (eg reduction of hospital-acquired infections); and the attitudes of the individual practitioner towards EBP (Titler and Everett, 2001; Cullen and Adams, 2012). Yet, existing approaches of EBP have been ineffective in facilitating its implementation (Greenhalgh et al, 2014).
Consequently, authors such as Cullen and Adams (2012) and Greenhalgh et al (2014) have called for a resurgence of the concept, especially concerning the components of EBP associated with involving patients in decision-making, and with expert judgement and experience. Greenhalgh et al (2014:3) consider it is time to return to implementing ‘real EBP’, where person-centred care is the priority, and health professionals and their patients ‘are free to make appropriate care decisions that may not match what best evidence seems to suggest’. Nonetheless, researchers including McSherry et al (2002), Epstein (2009) and Nevo and Slonim-Nevo (2011) have proposed an alternative, holistic approach to the application of evidence into practice, termed evidence-informed practice (EIP).
Journey towards evidence-informed practice
The problems with the uptake and effective implementation of EBP led to the emergence of the EIP concept. This concept is based on the premise that healthcare practice should, as a matter of principle, be informed by, rather than based on, evidence (Nevo and Slonim-Nevo, 2011). This implies that other forms of evidence (for example, patient experiences, the nurse's expertise and experiences), not just the ‘research evidence’, should be considered in applying evidence in practice.
McSherry et al (2002) defined EIP as the assimilation of professional judgment and research evidence regarding the efficiency of interventions. This definition was further elaborated as an approach to patient care where:
‘Practitioners are encouraged to be knowledgeable about findings coming from all types of studies and to use them in an integrative manner, taking into consideration clinical experience and judgment, clients' preferences and values, and context of the interventions.’
Nevo and Slonim-Nevo (2011:18)
It has been over two decades since EIP emerged in the literature, however, primary research on the concept has been limited. Hence, although the term EIP has gained momentum in recent times, the methods needed to implement it effectively are not widely known (McSherry, 2007; Woodbury and Kuhnke, 2014). While some proponents of EIP (eg Epstein 2011; Webber and Carr 2015) have identified significant differences between EBP and EIP, most researchers (eg Ciliska, 2012; Shlonsky and Mildon, 2014) have used the terms interchangeably.
Ciliska (2012), for instance, developed an evidence-informed decision making (EIDM) module, but referred to the steps of EBP (ie Ask, Acquire, Appraise, Integrate, Adapt, Apply, Analyse) as the processes to be followed in implementing EIDM. Ciliska (2012) explained that the term EIDM was adopted to signify that other types of evidence are useful in clinical decision-making and to attempt to get beyond the criticisms of EBP. This notwithstanding, the author maintained the existing process for implementing EBP. Similarly, Shlonsky and Mildon (2014) used the terms EBP and EIP interchangeably, as they consistently referred to an EBP approach as EIP. Examples include referring to the steps of EBP as ‘the steps of EIP’ (Shlonsky and Mildon, 2014:3) and referring to Haynes et al's (2002) expanded EBP model as a ‘revised EIP model’ (Shlonsky and Mildon, 2014:2).
Another term that is often used interchangeably with EIP is ‘knowledge translation’. This term has been explored extensively. For example, the Canadian Institute of Health Research (CIHR) has adopted knowledge translation to signify the use of high-quality research evidence to make informed decisions (Straus et al, 2009). The CIHR (Graham et al, 2006) developed a ‘knowledge to action’ model intended to integrate the creation and application of knowledge. The model acknowledges the non-linear process of applying evidence in practice, where each stage is influenced by the next, as well as the preceding, stage. In a typical clinical setting, the actual process of applying evidence in practice is not linear, as acknowledged by the proponents of EBP, but cyclical and interdependent. Ciliska (2012) linked Graham et al's (2006) model to the components of evidence-informed decision-making. According to Ciliska (2012:7), the knowledge-to-action model ‘fits with the steps of evidence-informed decision-making’. However, like EBP, the term ‘knowledge translation’, differs significantly from the EIP concept because it focuses on the ‘research evidence’ in decision-making.
The apparent confusion surrounding EIP is due to inadequate information about its components and the methods involved in implementing the concept. To foster a culture of EIP among health professionals, they must first be made aware of the actual components of the concept and the strategies involved in its successful implementation. The following section uses case scenarios to provide a description of the factors and elements of the EIP model and defines how it facilitates the application of evidence into clinical nursing practice.
Systems thinking
The clinical setting within which nurses work is a complex system made up of several interdependent and inter-related parts. Problems with healthcare delivery and management must therefore be perceived as a consequence of the exchanges between elements of the systems, instead of an outcome or the malfunctioning of a particular element. This, McSherry and Warr (2010), have referred to as ‘systems thinking’.
Effective implementation of EIP demands an understanding of the various parts of the system that come together to aid the application of evidence in practice.
The evidence-informed practice model
The original model
The earliest version of the evidence-informed practice model is depicted in Figure 1. This was developed specifically for nurses and was originally named ‘the evidence-informed nursing model’. The model presented in Figure 1 was developed through PhD research conducted by Robert McSherry (2007), with the aim to explore, through a mixed-methods study design, why the use of research as evidence in support of clinical nursing practice remains problematic. Study participants were registered nurses practising in a hospital trust located in north-east England.
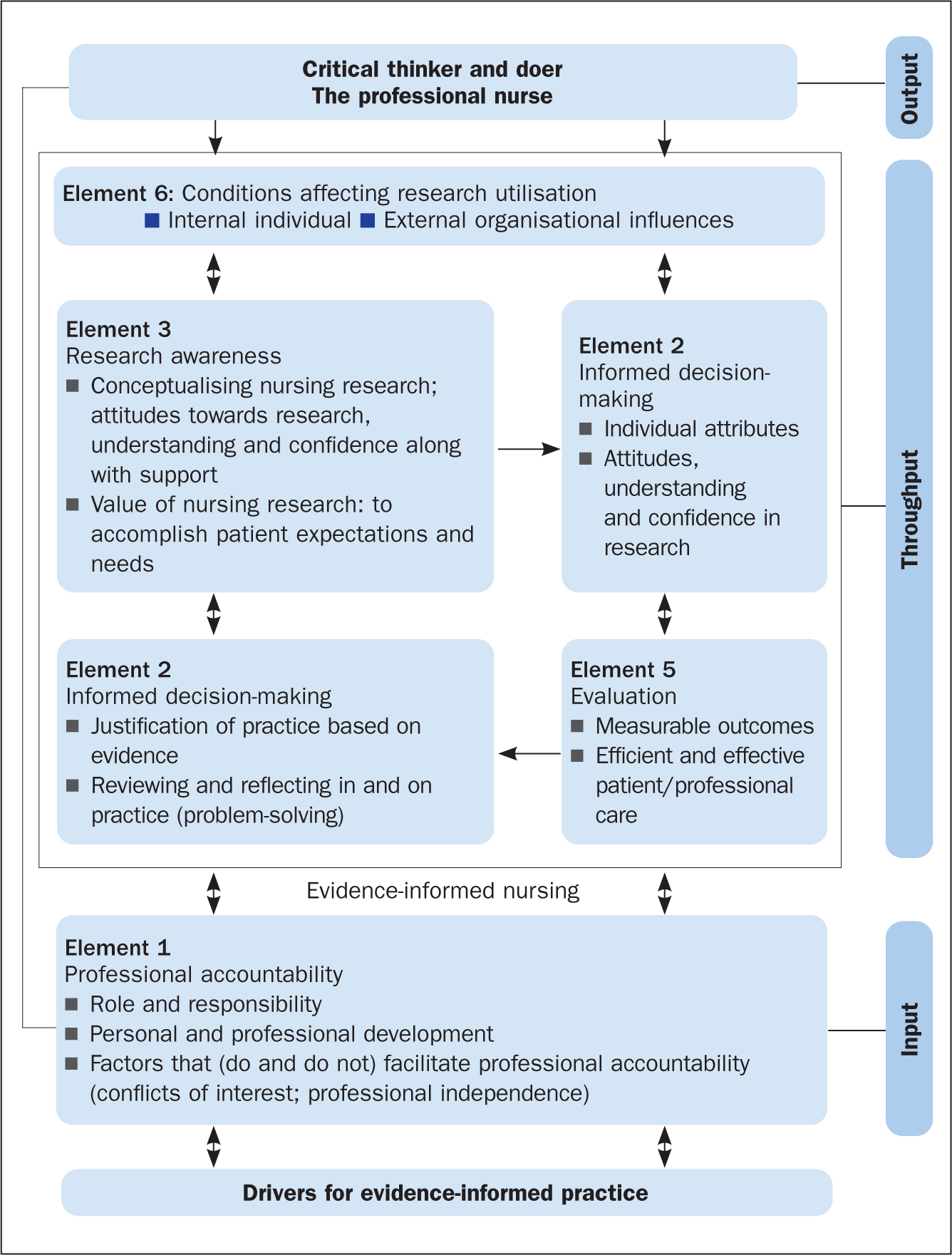
The results of McSherry's (2007) study showed that, to effectively apply evidence in clinical nursing practice, nurses needed to be informed of, and be able to interact with, several key elements. The evidence-informed nursing model was developed as an alternative framework for facilitating the application of evidence in clinical nursing practice and was grounded in the principles and practices of systems thinking. This is because, primarily, the model provided an integrated process to applying evidence into practice, consisting of:
- A clearly defined input; to encourage nurses to use evidence in practice
- Throughput; facilitation of the processes associated with the elements
- Output; improved standards of professional practice
The revised model
The evidence-informed nursing model has been adapted to the evidence-informed practice model. The new model (Figure 2) is adapted in several ways. First, it has been modified to be all-inclusive, so it could be applied to any health profession. Second, the model has been simplified to show the interconnectedness of the various factors and elements that enable a professional to use evidence in support of their clinical decision-making. Third, the model demonstrates the ongoing complexity that health professionals find themselves working in, in the quest to apply evidence to clinical practice. Last, the EIP model incorporates the principles and components of EBP, which is particularly evident in the EIP cycle (the throughput phase of the model).
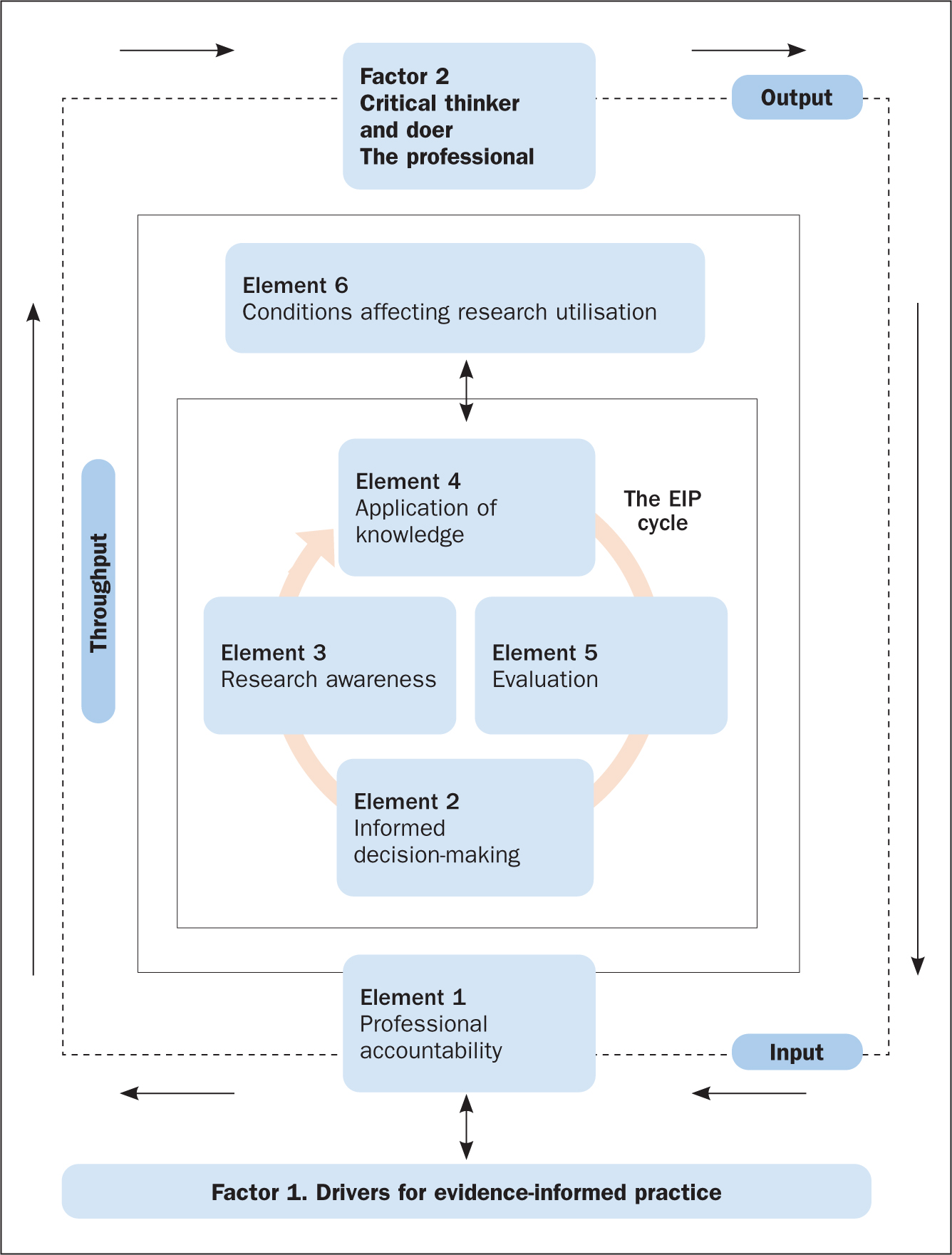
The factors and elements of the EIP model (Figure 2) are explored in more detail below with reference to two scenarios, which are used to apply the EIP model to clinical nursing practice within both a scientific and the wider context within which nursing care takes place.
Factor 1
The first factor of the EIP model is ‘Factor 1. Drivers for evidence-informed practice’ (Figure 2). In order for nurses to enhance patient care and experiences, along with improving their knowledge and skills of the patient's condition and associated signs and symptoms, they need to be aware of what EIP is, what it involves, and the principles required to make it happen. Applying the scenarios, it is essential that the nurse understands and can identify the key elements that drive successful implementation of the EIP concept. This is referred to as the drivers for EIP, which are illustrated in Figure 3 and discussed below.
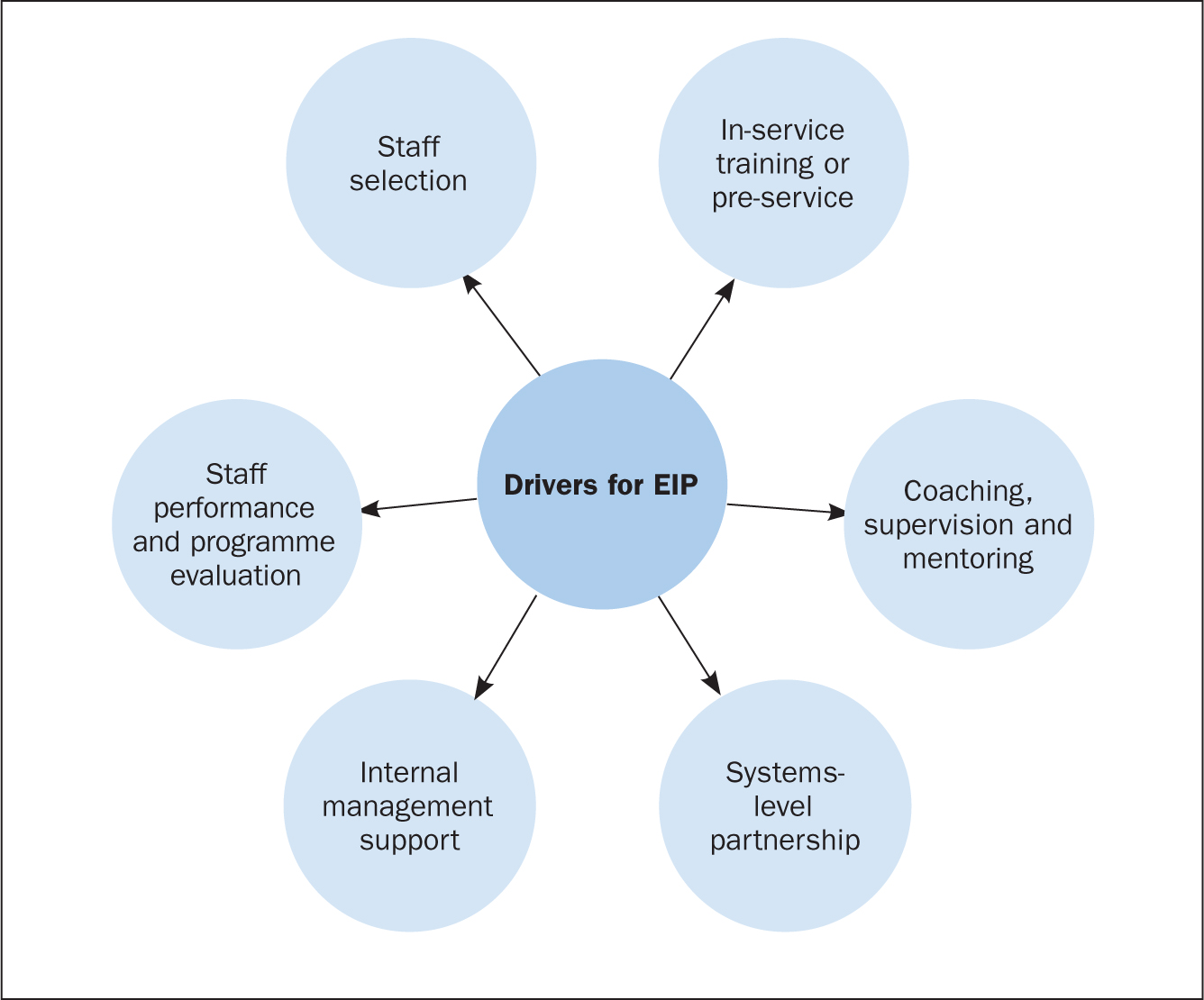
Drivers for EIP
Staff selection
Recruiting, interviewing and redeploying existing staff or hiring new staff are part of the staff selection process (Dill and Shera, 2012). The importance of this driver is to identify personnel who qualify to implement the EIP programme or model. Additionally, it aims at selecting individuals within the organisation (for example coaches, supervisors, and trainers), who will ensure that the required organisational changes to support nurses in the effective implementation of EIP are done.
In-service training or pre-service
Training on EIP programmes involves activities that are related to offering instruction, providing specialist information or skills development in a structured manner to nurses and other key healthcare staff involved in the EIP programme. Nurses, as well as other members of staff, must learn when, how, where, and with whom to use new approaches and skills in applying evidence to practice (Metz et al, 2007).
Coaching, supervision and mentoring
The coaching and mentoring approach enables new skills to be introduced to nurses on the ward with the support of a coach. The duty of a coach is to offer expert information and support, together with encouragement, opportunities and advice to practise and apply skills that are specific to the EIP programme. Effective implementation of human service interventions (such as EIP) requires changes in behaviour at administrative, supervisory and practitioner levels (Dill and Shera, 2012). Coaching and mentoring are the main ways to bring about a change in behaviour for staff who have been successfully involved in the beginning stage of the implementation process and throughout the life of the EIP programme.
Systems-level partnership
This refers to the improvement of partnerships with the broader and immediate systems to ensure access to required funds, and institutional and human resources necessary to support nurses' work. The immediate systems-level partnership refers to working with individuals or organisations that directly influence healthcare delivery (for example, nurses and doctors).
Partnerships within the broader system, on the other hand, refer to policymakers, funders or other organisations that may support the EIP programme, but are not directly involved in delivering health care. A variety of activities may be conducted as part of the development of systems-level partnerships to aid the implementation of EIP. These may include fundraising activities to support the implementation of EIP programmes, as well as the use of external coaches and consultants to assist with mentoring, technical assistance and training on an ongoing basis.
Internal management support
This involves activities that are associated with establishing processes and structures within an EIP programme to enhance effective implementation of the programme. This is necessary in order to inform healthcare decision-making as well as keep staff organised and focussed on desired care outcomes (Fixsen et al, 2005). Instances of internal management support include the formation of institutional structures and processes, the allocation of resources to support selection of suitable staff, and administrative support for efficient training.
Staff performance and programme evaluation
This involves evaluation of staff performance and the overall EIP programme to determine whether the objectives of the programme have been achieved. To do this effectively, it is important to evaluate the outcomes of the above-defined drivers, in particular, staff selection, in-service training, as well as coaching and mentoring. This will offer managers and stakeholders insight about the effectiveness of staff selection, training, and mentoring in facilitating the application of evidence into clinical practice (Dill and Shera, 2012).
Elements of the EIP model
The first element of the EIP model is professional accountability, depicted as an ‘input’ in Figure 2. This is an essential part of a nurse's roles and responsibilities and is reaffirmed in the nursing Code (Nursing and Midwifery Council, 2018) of professional practice, the contract of employment and job description. In both case scenarios involving Mitchell and Yvonne (Box 1), professional accountability is evident on several fronts: the nurse must establish a caring, compassionate and therapeutic relationship with the patients by involving and engaging them in shared decision-making regarding all aspects of their care, treatments, and interventions; the nurse is accountable and answerable to the patient and his or her professional colleagues throughout the patient's journey.
Box 1.Patient scenariosScenario 1Yvonne, aged 31, is admitted to the emergency medical unit following a visit to her GP for a non-healing wound to her right big toe. The GP also reported that Yvonne has had a recurring sore throat, extreme tiredness and a low white blood cell count.The GP requested an urgent investigation of these symptoms. Yvonne was placed in a side room for precaution.Scenario 2Mitchell, aged 58, arrives in the emergency department complaining of severe chest pain. He is diaphoretic (sweating excessively) and says his pain is radiating down his left arm and up into his jaw, and he adds that he feels nauseated. A few minutes after admission, he suffers a cardiac arrest.He is resuscitated and transferred to the intensive care unit. He is intubated, is placed on a ventilator and has a central line catheter in place.
Throughput: the evidence-informed practice cycle
The EIP cycle (located in the ‘throughput’ of Figure 2) involves the processes or methods through which nurses apply evidence in support of their decision-making in clinical nursing practice. This often occurs in a clinical nursing environment that is complex, constantly changing, and involves numerous members of the multidisciplinary team, patients and their family. Effective communication (verbal and written) is essential for ensuring that the various elements are interchanging, interconnecting and communicating between, and with, each other. For example, the case of Yvonne in scenario 1 (Box 1) can be used as an example to underline the importance of good communication. It is important to explain to the patient and her family the reason for nursing her in a side room rather than the main ward. In this situation, avoiding and preventing cross-infection is essential to safeguard Yvonne from harm.
To ensure the EIP cycle proceeds effectively requires that the nurse (the health professional) acts as the conduit for the interplay between the different elements of the model (ie Element 2: informed decision-making; Element 3: research awareness; Element 4: application of knowledge; and Element 5: evaluation). These elements will be further explored.
Element 2. Informed decision-making
This involves two-way communication between the nurse and the patient(s), and is critical in ensuring there is a robust relationship (honesty, openness, transparency) founded on the principles of person-centred care (McSherry and Warr, 2010). It reaffirms the ethical principle of a patient's right to make an informed decision about what is suitable for them, and takes into account their beliefs, values, priorities and personal circumstances. In case scenario 2, applying the EIP model, the critical care nurse will be expected to involve Mitchell's (the patient's) relatives, medical staff and other members of the healthcare team in making decisions about, for example, ventilator management and care of the central line catheter. However, decision-making in an intensive care unit can be complex, and some of the decisions may involve the nurse only. Similarly, applying the EIP model in case scenario 1, the nurse will be expected to communicate with the patient (Yvonne), carers and colleagues about the importance of hand hygiene, wound care and the importance of using precautions to avoid hospital-acquired infections when caring for the patient.
In both case scenarios, the nurse must endeavour to involve the patient/family members in the process of decision-making by providing them with timely, appropriate and relevant information needed to make often complex and life-changing decisions.
Element 3. Research awareness
This element refers to motivating practitioners to acquire skills and knowledge, as well as to conceptualise what research and evidence involves and the significance they have in improving standards of healthcare practice (McSherry et al, 2006). Research awareness is reliant on the nurse's attitudes towards research, the acquisition of knowledge and confidence about the value of research to practice, and on having supportive managers and colleagues.
This element of the EIP cycle, contained within the model, incorporates three of the steps (Research awareness) of EBP: ask a clinical question, search the literature for research evidence to answer the question, and critically appraise the evidence obtained). Although the nurse is not required to be a researcher to implement the EIP model effectively, they must be knowledgeable about relevant databases and search engines (such as Medline and Google), as well as critical appraisal tools, in order to be able to include high-quality research evidence when making patient care decisions.
However, the EIP model acknowledges the fact that research evidence may not always be readily available, and nurses may not have the necessary hardware and software in the care environment to enable them to search for research evidence. Hence, recommendations by Greenhalgh et al (2014) led to inclusion, within the EIP model, of nurses as critical thinkers and doers which, therefore, allows them to make appropriate care decisions based on patient preferences and actions, the clinical state, clinical setting and circumstances, and advocates that nurses apply their own knowledge, expertise and clinical experiences in clinical decision-making, which may not necessarily match what the research evidence seems to suggest.
With reference to scenario 2 (and similarly for scenario 1), to adhere to the EIP model the nurse would take the following steps:
- Update his/her knowledge about Mitchell's clinical presentation
- Search Medline for research evidence on ‘chest pain’, and ‘cardiac arrest’ and its associated symptoms. Based on the number of articles obtained, the nurse reads the titles and abstracts, and then, the full text of selected articles to exclude irrelevant articles. The remaining articles are then critically appraised to include the best research evidence in patient care decisions.
In situations where the above steps are not possible, the model advocates that the nurse endeavours to make the best care decisions possible based on patient preferences, clinical state, context and circumstances, and the nurse's own expertise and experience, as well as the experience of the patient and family members where possible.
Element 4. Application of knowledge
This is a complex element that requires the gathering and assimilation of various sources of information, evidence, quality and standards, and policy and guidance, to support the nurse's decision-making in clinical practice. In relation to both scenarios, the nurse would need to:
- Apply knowledge acquired from the patients (Mitchell and Yvonne), along with information from their relatives
- Apply evidence from reviewing the findings from research
- Take into account information gleaned from engaging with the multidisciplinary team
- Ensure they follow recommended local and national guidance and policy on the management of each patient's condition.
It is imperative that the nurse is experienced, knowledgeable, and competent in order to make the most appropriate care decisions together with the patient, the family and the wider multidisciplinary team. To do this effectively, the nurse requires certain personal attributes, it is also important for the organisation within which the nurse works to have specific institutional characteristics. Institutional features include culture, education and training, and workload/skill mix, whereas personal characteristics include improved confidence, attitude, understanding and behaviour towards the application of evidence into practice.
Element 5. Evaluation
This element of the EIP cycle within the model measures the effects of decision-making and actions of the nurse on care outcomes and in creating an optimal care environment. In both scenarios, the nurse would need to periodically evaluate specific processes and outcomes of care. For example, with regards to scenario 2, this would include:
- Monitoring how Mitchell is performing on the ventilator
- Taking the necessary infection prevention precautions to avoid the development of infections related to the insertion of a central line and transmission of hospital-acquired infection
- Monitoring improvement in Mitchell's general wellbeing.
Depending on the outcome of the evaluation, Mitchell's care plan would be either revised or continued.
Element 6. Conditions affecting research utilisation
Research utilisation involves critically appraising research findings, disseminating, and using the knowledge obtained from research to cause changes in an existing healthcare practice (Titler et al, 1994). The conditions that affect research utilisation are grouped into five domains (Wang et al, 2013):
- The process involved in utilising research findings
- Accessibility to research
- The quality of research
- The knowledge and attitudes of the nurse (health professional) regarding the use of research findings
- The organisation within which the findings of research are to be implemented.
In the two scenarios (Box 1), the nurse needs to be aware of the potential barriers to research utilisation and identify ways to overcome these in order to effectively apply evidence to healthcare practice. In addition, the clinical environment within which nurses work must provide sufficient support in order to enhance the effective and consistent application of evidence to practice. Nurses must be supported to acquire the necessary knowledge, skills, and understanding needed to practise safely (ie competently and confidently). In addition, the resources necessary to obtain research evidence, such as IT (computers and internet), must be readily available in the clinical setting for easy access to information.
Factor 2 (Output). Critical thinker and doer, the professional nurse
To ensure that nurses inform their decisions with the best available evidence, it is imperative that they have a sound understanding and knowledge of what constitutes the EIP model (Figure 2). Successfully engaging with the various factors and elements of this model will lead to the desired outcome—that of a professional who is a critical thinker and doer, a professional nurse who, as argued by Brechin (2000:44), is ‘knowledgeable and skilled, yet welcomes alternative ideas and belief systems, appreciating and respecting alternative views’. In this context, it is about creating a caring and compassionate environment in which excellence in nursing practice occurs. This can only be exemplified by ensuring that decisions and actions are based on the best available evidence.
The benefits of the EIP model for the nurse, patient and family are that it simplifies a highly complex series of systems and processes pertaining to how evidence is used to support decisions made in clinical practice. The EIP model simply illustrates the why, the how and the sequencing of getting evidence into clinical practice. It also complements the evidence-based movement by offering a holistic systems-based approach to facilitating the application of evidence into clinical practice.
Conclusion
EIP is a holistic integrated approach to applying evidence into practice, which incorporates the steps of EBP within its system and processes. In other words, EBP is a subset of the EIP model, made explicit within the EIP cycle. Thus, EIP is neither an alternative to, nor a replacement for, EBP. The EIP model provides a framework for nurses (indeed all health practitioners) to deliver clinically effective care and enable them to justify the processes used and the service provided by referring to reliable evidence. Using two scenarios, this article demonstrated how the EIP model can be applied to clinical nursing practice. Future initiatives should focus on developing EIP educational interventions and determining the effects of such interventions on healthcare students' knowledge of, and attitudes towards, the application of evidence to practice.
KEY POINTS
- Two main concepts have been associated with the application of evidence into practice: evidence-based practice (EBP) and evidence-informed practice (EIP)
- The main feature that distinguishes EIP from EBP is the processes used in implementing the concepts
- EIP provides the mechanisms or processes to follow in implementing EBP
- EIP is not a substitute or replacement for EBP. EIP is an integrated approach to applying evidence to practice, which incorporates the steps of EBP in its processes
CPD reflective questions
- Make a list of the challenges you encounter in implementing EBP
- Use the same list and indicate how these challenges prevent you from using evidence to support your nursing clinical decisions and actions in practice
- How does viewing health and healthcare delivery as a complex system impact on your patient care?
- Make a list of the drivers that are encouraging you to support your clinical nursing decisions and actions with evidence
- Using your own experience to date and the information presented in the text, make a list of why and how you think evidence-informed practice forms part of your professional accountability and professional registration


