Clinical supervision, ‘a formal process of professional support, reflection and learning’ (Butterworth, 2022: 20) is an internationally recognised professional practice that can achieve benefits for the organisation, patient services and the providers of health and social care (Rothwell et al, 2021). Clinical supervision is well regarded in the literature as a supportive platform for nurses to reflect on and develop their practice (Masamha et al, 2022) and an evidence-based means to improve the effectiveness of care (Snowdon et al, 2017). Multiple models and frameworks of clinical supervision (Zonneveld et al, 2024) and varied modes of delivery (Gill-Meeley et al, 2024) have been developed and researched, including Wallbank's model of restorative clinical supervision (Wallbank, 2016); an established approach to support the emotional needs of staff. In recent years, clinical supervision has gained recognition as an integral part of professional healthcare practice and support (Cosgrove and Ashcroft, 2025), with increased prominence in contemporary nursing heightened by workplace pressures and the unprecedented challenges of the COVID-19 pandemic (Jones, 2023).
First launched in England in the post-COVID recovery phase (May, 2021), the professional nurse advocate (PNA) A-EQUIP (Advocating and Educating for QUality ImProvement) model is a relatively new initiative in nursing. A-EQUIP stems from Proctor's (1987) model of clinical supervision, essentially comprising the four functions outlined in Figure 1.
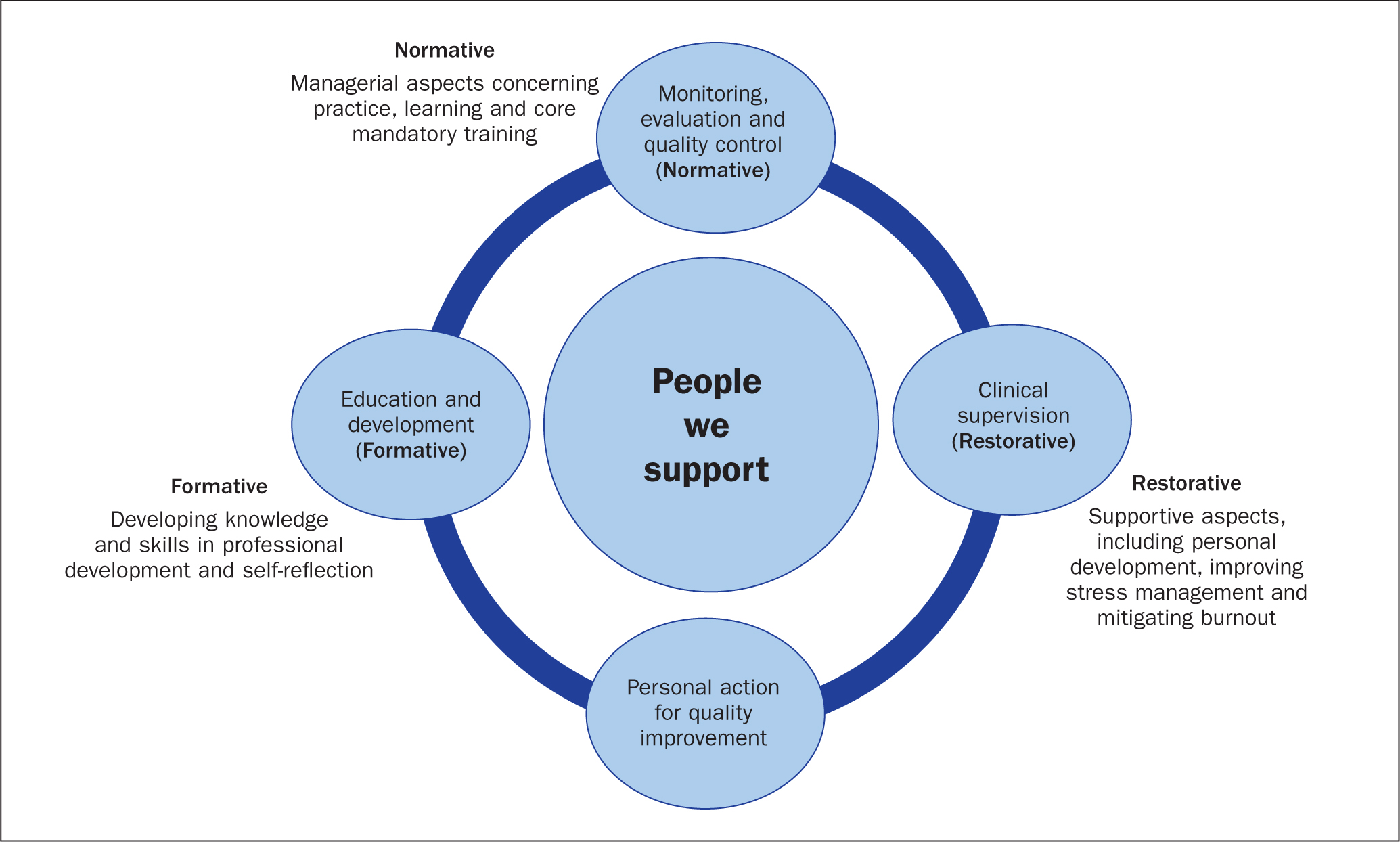
The PNA is defined as ‘a professional clinical leadership and advocacy role introduced to deploy the A-EQUIP model’ (NHS England, 2024). A national programme of PNA training (NHS England, 2024) and associated standards for education and programme delivery (Royal College of Nursing (RCN), 2023) are designed to enable registered nurses (RNs) to competently fulfil the role. Duties of the qualified PNA are to facilitate and support reflective conversations and to foster a culture of restorative learning from experience in a way that critically examines and improves nursing practice and care.
Background
Research relating to the role of the PNA is in its infancy. Apart from two research studies (Lees-Deutsch et al, 2023; Smythe et al, 2023), post-implementation evaluations of this model currently comprise anecdotal accounts. From the viewpoint of project leads and practising PNAs, supervisees are seen to benefit emotionally through skilled restoration in a safe reflective space, and early informal feedback suggests promising positive impacts (Mahachi, 2020; Griffiths, 2022; Wales and Dillon, 2022; Hogan, 2023; Wade, 2023; Topping and Gamble, 2025). Brief organisationally situated case studies also provide evidence of creative initiatives to improve physical and/or mental wellbeing, boost staff morale, and resolve disclosed stresses and concerns (NHS England, 2025a).
A national evaluation of the PNA programme in England was reported in 2023 (Lees-Deutsch et al, 2023). In this mixed-methods study, participants disclosed a range of positive benefits for individual nurses receiving restorative supervision, plus benefits for patient care and service provision. The PNA training programme also opened an opportunity to engage in further study and continuing development thereafter. The authors recommended further research to clearly articulate the benefits of the PNA programme to individuals and teams, over time.
Smythe et al (2023) used qualitative methods to explore the realities of the PNA role and associated use of the A-EQUIP model in practice. In this single-site study, the restorative function of A-EQUIP took precedence, and reciprocal support was considered important to the welfare of the PNA. It was identified that outcome data were difficult to capture and define, and further research was recommended to provide a deep and shared understanding of impacts. In reviewing the interview data derived from this study, the researchers recognised an opportunity to further understand and evidence the self-perceived personal and professional impacts through secondary qualitative research. The study was funded by NHS England/NHS Improvement and carried out over a 4-month period from December 2023 to end March 2024.
Study design and methods
Interview data derived from an interpretive descriptive study with qualified PNAs (Smythe et al, 2023) was subjected to qualitative secondary analysis (QSA); a methodology designed to investigate a new research question using pre-existing data (Heaton, 2004). QSA is said to have several advantages, including maximum use of publicly funded research, additional evidence-based findings on the same topic without the need to further recruit or burden the population of interest (Beck, 2023), and a resourceful alternative to primary research in terms of time and costs (Kelly et al, 2024). These benefits appeared valuable to the researchers in a climate of nursing workforce pressures (RCN, 2022), reported challenges in research funding (Farquharson, 2024) and a need for timely evidence of the perceived impacts of an innovation in practice.
The aim of the primary study was to obtain firsthand accounts of preparation for, and experiences of, the PNA role, and the perceived influences of new supervision practices. Qualitative data were gathered from 17 trained PNAs based in a combined acute and community NHS Trust in the Midlands. Data were collected between November 2022 and January 2023. Participants had a minimum of 3 months' experience in the PNA role at the time of recruitment, and a majority were female RNs. Semi-structured, audio-recorded interviews were held either face-to-face in-person or online remote. A topic guide of questions was used to elicit participants' perceptions and experiences in keeping with the study aim. All interviews were transcribed verbatim by a professional transcription company. The transcripts were coded 01-17 to protect the identity of the study participants, and to provide assurances of anonymity and confidentiality.
Secondary research question
What are the self-perceived personal and professional impacts of educational preparation for, and performance in the role of, PNA?
Working definitions
The following working definitions provided a common understanding of the meaning of impact in the context of this study:
Ethical considerations
The primary study was approved by the UK's national authority for regulating research, the Health Research Authority (ID:316718), and agreement was obtained from the Research and Development (R&D) Directorate of the participating research site. All interviewees provided written informed consent in advance of a research interview and were given written assurance of confidentiality and anonymity of all data. The lead and co-researcher of the QSA were principal investigators for the primary research, and therefore custodians of the data. Prior to commencing the secondary study, the researchers received confirmation that no additional approvals were required to carry out the QSA (HRA and R&D Directorate, email correspondence dated 6/11/23 and 30/11/2023 respectively).
Qualitative secondary analysis
Transcripts from the primary study were re-analysed using conventional qualitative content analysis (Hsieh and Shannon, 2005); a method suited to the analysis and interpretation of textual data, particularly when existing theory or research literature on the topic is limited. This was supplemented by a hands-on-guide to support the analytic process (Erlingsson and Brysiewicz, 2017). Each step of the analysis moves from lower to higher levels of abstraction; from the manifest and literal content, to interpreted latent meanings (Figure 2).
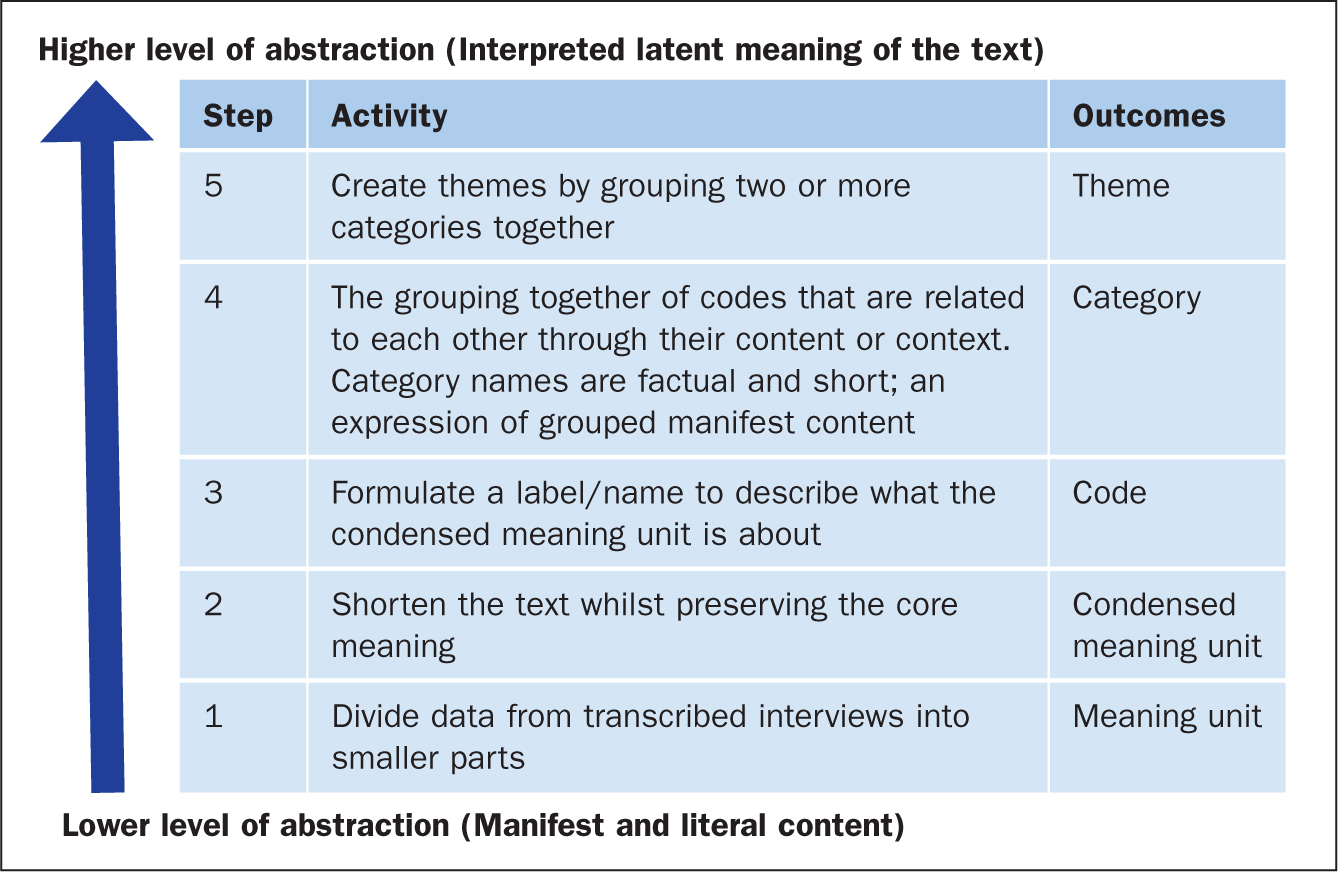
Steps 1 and 2
Two researchers (WW, AS) independently analysed each transcript, using a selective highlighting technique. A table for each interview transcript was developed, with respective columns to accommodate extracted text data (meaning units) and condensed meaning units. Each condensed meaning unit was further analysed to determine if the text data represented a personal or professional impact of becoming or being a PNA, and whether conveyed in a positive, negative or neutral tone. A consensus meeting was held to compare, discuss and agree the emergent findings.
Step 3
One researcher (WW) independently coded each condensed meaning unit, all of which were subsequently reviewed by a second researcher (AS). An independent review of a small sample of the coded extracts was undertaken by two experienced qualitative researchers who were members of an external reference group to the study (LLD, RK). Consensus was observed for the majority of codes, and facilitated meetings were helpful for discussing individual reactions to the text and possible alternative interpretations. Examples of analytic steps 1-3 are presented in Table 1.
| Line no. | Meaning unit | Condensed meaning unit | Code | Personal/professional impact code |
|---|---|---|---|---|
| Transcript 2 | ||||
| 699–703 | ‘Are you doing your manager's job? Are you doing a PNA? And I'm always saying that actually, you can't take the two hats off. I'm like … What's that man with the many hats? They're just on top of each other’ | Many hats | Role conflict | Personal impact on self (neutral) |
| Transcript 4 | ||||
| 94–6 | ‘… sometimes it becomes really overwhelming, listening to people speaking if they are really distressed’ | Overwhelming | Overwhelming | Personal impact on self (negative) |
| Transcript 7 | ||||
| 1415–6 | ‘I would just say that it's really, really rewarding [PNA role]. I find it such a rewarding part of my job’ | Really rewarding | Rewarding | Personal impact on self (positive) |
| Transcript 8 | ||||
| 90–2 | ‘It [PNA course] made you think about the way you approach emotion, the way you approach people and resilience more widely’ | It made you think | Critical thinking | Personal impact on self (positive) |
| Transcript 14 | ||||
| 39–43 | ‘We … recognised that there was a need for … more supervision … having that [PNA A-EQUIP] as a very structured model was seen as a positive way forward’ | Having a very structured model | Provided structure for supervision | Personal impact on others (positive) |
Step 4
Coded meaning units were formed into categories based on related content (WW). Each category was given a short factual label to provide context and meaning to the findings within. In this study, categories were chosen as the highest level of abstraction due to the researchers' intention to use the secondary findings to form preliminary items for a ‘PNA Personal and Professional Impacts’ survey questionnaire for meaningful understanding and consistency in evaluating the impacts of the PNA role within and across organisations. All members of the analytic team (WW, AS, LLD, RK) agreed on the suitability of the grouped codes and category labels.
Findings
A total of 183 codes were developed from the data. The majority of codes described the personal (n=75) and professional (n=76) impacts of being a PNA. The remaining 32 codes described impacts of becoming a PNA: personal (n=25)/professional (n=7). When grouped, these formed 19 categories (Tables 2and3).
| Personal impacts (on self) | Professional impacts (on others) |
|---|---|
|
|
|
| Personal impacts (on self) | Professional impacts (on others) |
|---|---|
|
|
Five of the categories in Table 3 contained coded meaning units that conveyed perceptions of positive impacts and isolated neutral responses. Four categories (denoted by an asterisk) contained accounts of impacts that were voiced in a negative or neutral tone and spoke of personally experienced conflicts, insecurities, consequences and challenges in the role of being a PNA.
Becoming a PNA: personal impacts on self
Participants equated the PNA training programme with learning opportunities, including new knowledge and academic skills at a higher level of study and associated benefits such as shared learning experiences, professional networking, and affirmation of existing abilities. In general, PNA preparation was an apparent mixture of personal challenge and reward that primarily equipped nurses for the role, but also inspired continuing professional development:
‘I think it was just nice to do something different … probably a little bit out of my comfort zone … It was just so good … I'm going to keep learning as long as I can.’
Preparation for an advocacy and empowerment role was reflected in accounts of learning to listen, signpost and encourage self-direction, together with the development of critical thinking and reflective practice skills, and increased self-awareness:
‘I think you learn a lot about yourself and how you react to things as well in different situations.’
Becoming a PNA: professional impacts on others
Many of the participants regarded the PNA role as beneficial to the nursing workforce by way of formalising existing structures for clinical supervision and support in practice. The findings suggested that aspects of the PNA role already featured in the work life of some participants, and many appeared to welcome the endorsement of existing approaches to supervision and support:
‘To have more knowledge on how to support my team … more equipped for the support that you can provide, to make it all official … a more structured way to support your colleagues.’
‘I kind of feel I was supporting them in that kind of way and what we do anyway … I suppose just to kind of formalise it.’
Being a PNA: personal impacts on self
The findings suggested that participants enthused, embraced and endorsed the PNA role, championed the model and overcame some scepticism as a consequence of being a PNA:
‘I was quite sceptical about the process because I thought it was another do-gooder thing that was taking place. But I've really sort of been on-boarded with the process.’
There was a general sense of satisfaction, enjoyment, fulfilment and reward attributed to the PNA role, particularly in relation to the observed positive impacts of staff support and restoration. Success stories were identified by some as personally encouraging and motivational with regard to the role. Participants spoke of making a difference, recognising the potential to bring benefits, and conveyed a sense of authentic pride:
‘So, it's knowing that that support's there, being part of that support … I'm quite proud of that.’
Personal gratification was also apparent in examples of emotional gain and consolation from supporting others, and in personal feedback and ‘thank you’ messages from trainees and supervisees:
‘The biggest motivation I get is basically seeing them coming back to work … and saying “thank you very much for the support”, “thank you for listening”.’
Participants suggested their nursing skills and abilities were enhanced in a number of ways in the PNA role, including role extension, transferable advocacy skills, teamwork and collaborative working. Four PNAs had become a mentor or educator to prepare trainee PNAs, and their accounts conveyed a sense of personal progression, achievement and enjoyment. Active listening skills and respectful responses were explained as skills that developed with experience, together with confidence and competence to undertake the PNA role. Examples included learning to listen, to accept silences and to self-regulate behaviour:
‘I don't jump in and give advice like I used to … Usually I'd go, “what about this?”, but it's not to help me, it's to help her. It's all about her and how she needs to progress in her professional life.’
In contrast, participants experienced communication challenges mostly related to listening (which could be intense), silences and holding back opinion. There were some personal insecurities and doubts about role performance, and feelings of being ‘overwhelmed’ (PNA 02) or for situations to become ‘overwhelming’ (PNA 04). Recollections of poignant supervision scenarios depicted exposure to personal, distressing, difficult and demanding issues with emotional consequences:
‘… It felt really intense listening to somebody and … and just thinking they are going through that, so even when I got home, I was still feeling really some of it.’
One participant described the PNA role as ‘not easy … a challenge’ (PNA 05), and various sources of conflict were experienced by participating PNAs. These included conflicting demands on work and personal time, PNA role/professional boundaries, personal conflicts of interest, a perception of intra-professional suspicion and role conflict which was by far, a commonly expressed concern:
‘And sometimes I don't recognise it as restorative supervision … I just recognised it as being part of my job. It just feels like, “Actually, this is me being your team leader and supporting you.” … It is hard.’
Being a PNA: professional impacts on others
Participants saw the PNA role as providing a haven for workplace support. This was reflected in accounts of being approached for advice, and the availability of a resource to provide needs-based support. There were suggestions of the PNA being approachable; a trusted confidante who offered a safe space for staff in need of an outlet:
‘She said you are the first person that I've told … and it was bothering her, but she never said it … I think she never said it to anybody because she didn't trust people.’
‘Sometimes … you don't know how that other person is feeling, unless they really express it … that safe space of restorative supervision made them able to express what they were feeling.’
Restorative supervision was perceived as helping to develop individual's reflective understanding of a situation, from which fresh perspectives or further issues may come to light. Self-determination and creative thinking were apparent principles of supervision to facilitate personal problem-solving, however with the caveat of guided support and signposting:
‘But also, that solution focused, turning it round and sort of asking them how they think this can be improved.’
‘Sometimes we signpost … Signpost them to wellbeing services … to get support or occupational health self-referral or have a conversation with a manager.’
PNA supervision sessions were viewed as a catalyst for change. The following quotes provide examples of perceived positive outcomes for supervisees: a personal change ‘for the better, not for the worse’ (PNA 11) and a satisfactory conclusion ‘that this is the time to move on’ (PNA 06). In relation to the latter, career conversations were a feature of many exemplar supervisory sessions, primarily as a consequence of, as opposed to a reason for, accessing support. Wider organisational change was also apparent in examples of practice development, service and care quality improvement projects, with reference to A-EQUIP or as a natural outcome of supervision:
‘… So, we completely redesigned the [surgical pathway] booklet, introduced the safety brief… Massively improved documentation, because I then went back and audited it again, so we'd got like 100% compliance.’
‘… as a team leader, and a supervisor, you do also need to … with their [supervisees] permission, be able to instigate a little bit of change from that’
The perceived contributions of restorative clinical supervision to safe and effective clinical practice were also apparent in participants' accounts of related opportunities for learning and education, either as individuals or to support organisational action plans:
‘Sometimes when something goes wrong … as long as … you learn from it and you try and keep your patients safe.’
‘Obviously, there is that thing of how are we going to address that learning gap? … As a PNA I have to put that feedback to the education team; these are the things that have been highlighted during [PNA sessions] …’
Numerous accounts of restorative supervision contained synonyms that depicted nurses' emotional wellness after their participation in restorative clinical supervision. Examples include ‘happier’, ‘feeling/getting better’, ‘less stressed/angry’, ‘calmer/more relaxed’, ‘reassured’, and ‘doing well’. Accounts of PNA supervision having influenced retention and absence from work were also apparent in the findings, and professional relationships were fed back as being improved, and in one instance, thought to be developed through supervision:
‘She was saying that it's the first time in her career she's really thought about leaving the profession before retirement. Just leaving, just abandoning it and just getting out, whereas on the second session, she said she'd felt like she'd been able to work through things and she actually said; “I am dealing with the issues now, rather than feeling like I have to run away from them”.’
‘… We've got a good relationship which is nice, I think probably sooner than we would normally have done because of the PNA sessions … so that's really positive.’
Confidential supervisee feedback was sought by the organisation, but it was apparent that some chose a more personalised approach directly with the PNA via email or in-person. The findings depicted the PNA role as a valued source of support, appreciated and of benefit to the nursing workforce. Participants recalled supervisees perceptions of a positive experience; better than expected, of being inspired to train to be a PNA, beliefs that they found it good to talk, felt valued and listened to and were pleased to be supported:
‘… They're happy with the fact that I've taken the time to sit down, have a session, train them, give them the support that they need, look at ways to make a plan.’
Discussion
This secondary qualitative analysis investigated the personal and professional impacts of educational preparation for, and performance in the role of a PNA, as perceived by practising PNAs. A wide range of impacts were revealed and thematically organised to represent the realities of becoming and being a PNA. As with any new initiative, evaluation data is important to evidencing the impacts of innovation and organisational responsiveness to change. The findings provide an insightful understanding of nurses' contribution to restorative supervision in the workplace, amid consistent concerns about the mental health and wellbeing of nurses (Kinman et al, 2020; RCN, 2024) and persistent nursing workforce challenges in the post-pandemic world (Kurtzman et al, 2022). First introduced in the aftermath of COVID-19 and in response to known adverse psychological effects on registered and trainee nurses (Couper et al, 2022), the PNA programme in England offers the opportunity to enhance workforce wellbeing, resilience and retention (Handley, 2024), and, as determined within the findings from this study, provides a structured approach to creating and enabling a supportive environment for restoration and recovery (Scanlan and Hart, 2024).
It has been suggested that person- and relationship-centred care provides the bedrock of professional practice in a nursing context (Ryan, 2022). This was reflected in participants' accounts of the PNA role, which espoused a commitment to personalisation and empowerment for successful restorative supervision. Discussions centred on the individual and their needs, reflexive learning, self-determined solutions and guided support to presenting professional or personal matters. The art of listening was an often-mentioned challenge yet acknowledged as important to developing an empathic understanding of supervisees' perspectives, feelings and thoughts. However, perceptions of negative personal impacts were positively reconfigured as PNAs developed their capabilities in mastering the skill. This finding serves as an example where, consistent with national findings, PNAs transitioned and adjusted their behaviours as they experienced the PNA role (Lees-Deutsch et al, 2023).
There has been much debate about the practice of restorative clinical supervision in nursing (Butterworth, 2022), the factors contributing to its effectiveness (Rothwell et al, 2021), and its various forms (Driscoll et al, 2019; Gill-Meeley et al, 2024). It was therefore encouraging to identify mostly positive impacts attributed to the new PNA A-EQUIP model, including improved staff wellbeing, reflective learning and professional development, staff retention and new career paths. Notable beneficiaries extended beyond the supervisee, as shown in examples of initiatives in education and practice for the wider benefit of patients and staff, and a range of rewards for the PNAs themselves. As a level 7 accredited training programme, the PNA role presented opportunity for academic, personal and professional achievements and gains. The researchers detected a commitment to, and belief in the advocacy role, and a genuine pride in the shared stories of successful outcomes for self and others. However, the reality of ‘being’ a PNA contrasted with the ‘becoming’ in terms of the experienced personal conflicts, insecurities, consequences and challenges. These findings invite reflection on the nature and quality of preparation to practise as a qualified PNA.
In the primary research (Smythe et al, 2023), mentorship from experienced PNAs, hands-on experiential learning in practice, opportunities to observe PNAs and simulated experiences were notable learning strategies that may be helpful to improving RNs' transition into the PNA role. The notion of work-based learning and practice-oriented learning outcomes also featured in the recommendations of a national evaluation of the PNA programme in England (Lees-Deutsch et al, 2023). The reality of the PNA role in practice draws attention to the importance of support for the PNA within respective organisations, and via external networks (NHS England, 2025b) in nursing fields of practice.
Strengths and limitations of the work
A particular strength of this study was continuity in the research process by the same two researchers who carried out the primary study. However, the available data were not collected to specifically address the QSA research question, which placed limits on the number of meaning units extracted for further analysis. Care was taken to reject potential findings in the absence of explicit understanding of the participants' responses to answer the QSA research question.
Erlingsson and Brysiewicz (2017) recommended researcher triangulation as a strategy for ensuring the trustworthiness of qualitative research. In this study, designated roles for four experienced qualitative analysts minimised the potential bias of a single analyst (Arias Valencia, 2022), thereby enhancing the credibility of the QSA findings by employing essential measures (Ahmed, 2024). Divergent personal reactions to the same phenomenon of study were observed and addressed through collaborative and respectful critical discussion, and by returning to the raw transcript data to inform ultimate decisions. Although the process of analysis followed a linear progression (steps 1-4), the transcripts were frequently revisited, and the outcomes of preliminary analysis reworked to provide an accurate and clear representation of the manifest content in the narrative text.
Participants in the primary study were recruited from a single research site. It is therefore possible to hypothesise that the self-perceived impacts of becoming and being a PNA could differ in alternative contexts of care. This supports further exploratory inquiry with a wider sample of PNAs based in alternative healthcare organisations and localities.
Conclusion
The qualitative secondary findings derived in this study strengthen the case for organisational use of A-EQUIP in the workplace and help to showcase the significant contribution of the PNA role to staff wellbeing, education and quality improvements in care. PNAs and their supervisees, together with the providers of nursing services, professional educators and policy makers play a collective role in influencing the impacts of the PNA A-EQUIP model and its future contribution to nursing and patient care. Regard for the welfare of PNAs must be reciprocated in practice and the impacts of preparation for, and performance in the role more deeply understood. Future inquiries could meaningfully contribute an evidence-base of effective interventions for PNA continuing professional development and support consistent with the normative, formative and restorative functions of A-EQUIP. Investigating the wider impacts on service provision, as perceived by the recipients of healthcare, is a further important workstream of evaluation research.


